The world salutes four Israeli scientists
In a world of supermodels and instant stars we’ve almost forgotten there are other cultural heroes. Four Israeli doctors and scientists won awards and received international recognition. Here's why
Puts the smile back on your face
Every year Newsweek magazine chooses 10 medical departments in the world to be awarded the title “Center of Excellence”. These departments attract patients from all over the world. This year, Dr. Eyal Gur, head of the microsurgery unit at Ichilov hospital, was selected by the magazine as one of the world's best microsurgeons.
Behind the microscope:
“Our unit focuses almost exclusively on removing bone tumors. Until a few years ago, in order to remove a cancerous growth we needed to sever the leg or arm. Microsurgery allows us to remove only the segment of the bone that is affected, and replace it with a healthy piece of the bone from elsewhere in the body.
“Yet I am most proud of a surgery that restores movement to people who suffer from facial paralysis, be it from birth, cancer or from a viral infection that causes nerve damage. The problem is not only aesthetical, but functional too; smiling, speaking and eating become quite difficult.
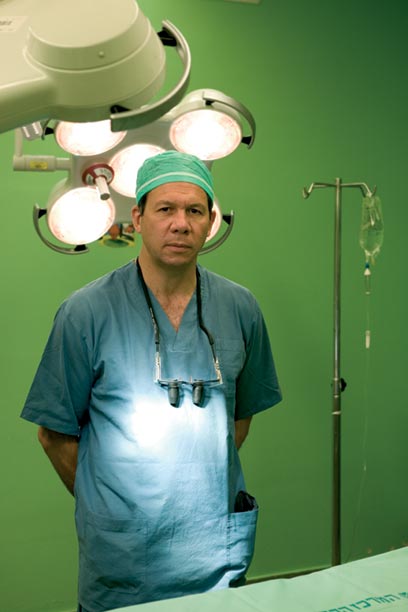
Dr. Eyal Gur (Photo: Yanai Yechiel)
We perform two operations; first, we implant a nerve from the leg into the healthy side of the face to act as an ‘extension cord’ which connects to the paralyzed part of the face. Six months later, once the nerve has reached the paralyzed cheek, we remove a tiny thigh muscle and connect its blood vessels and nerve endings to the transplanted nerve in the healthy cheek. After an additional six months, the patient can smile.
I consider this the highest expression of innovation and ingenuity in the field of microsurgery”.
The beginning
It all started with a young Palestinian who suffered facial injury after being involved in a car accident. The complicated operation which Dr. Gur performed on the young man's face was a success. One year later he has full control over his facial muscles.
The story of an Israeli doctor, who restored the face of a Palestinian boy, touched the hearts of the editors of ‘Newsweek’ and found its way to the pages of the magazine.
Dr. Gur, who suffered a severe injury while in combat during the first Lebanon War, told Ynet: “We put our hearts and souls into every patient, without discriminating. Before my injury, I had no political ideals, but now I believe in peace at all costs. I am not politically active because my work is very consuming, but if I am able to do something to bridge the gap between the two sides, then that’s my small contribution to peace.”
Sniffing out cancer
Dr. Hossam Haick, a lecturer and researcher in the Faculty of Chemical Engineering and in the Russell Berrie Nanotechnology Institute at the Technion - Israel Institute of Technology, invented an electronic nose which can diagnose cancer. An invention that won him a 1.73 million euro grant from the European Union.
Behind the microscope:
“When I was in medical school one of my friends was diagnosed with cancer. His illness got me thinking about developing tools to help diagnose and treat cancer. Electronic noses have been around since the 1980s but they were very big (about the size of a small fridge) and very expensive but not very accurate. I envisioned a smaller, cheaper device (about $500-$1000).

Dr. Hossam Haick (Photo: Yanai Yechiel)
"I researched the subject and heard about the EU grant two weeks before the closing date for submittals. I worked like crazy for those two weeks writing up the proposal.
“My olfactory system can diagnose cancer by analyzing a person’s breath. It is able to distinguish between the different types of cancer and infers what stage cancer it is. The ‘nose’ looks like a cellular phone with nano-size sensors and an electronic brain. The patient blows into the nose through a small pipe and the result is seen immediately on the screen. The sensors’ minute size – less than 100,000th of a hair – makes them extremely sensitive and thus are able to ‘smell’ the changes in the chemical composition of the exhaled breath, detecting the different characteristics of cancer. One can program the nose to sniff any given odor in the world.
“Cancer is usually detected at the third stage of growth (out of five stages). At this stage a tumor has already formed. Statistics show that when diagnosed at this stage, the recovery rate after five years from the time of diagnosis is only 15%. The electronic nose can detect cancer at its very first stages when there are only a few cancerous cells, thus ensuring a survival rate of up to 90%".
Dr. Haick received the Marie Curie Prize for Scientific Excellence. The grant is awarded by the European Union in an effort to encourage young promising scientists. This is the first time an Israeli won this award.
"I was happy when I heard of I had won, but then I realized the huge responsibility that's on my shoulders. That's why I work around the clock. I bought equipment with the prize money, and I’m building a team of scientists from Israel and abroad.
Tissue engineering
Dr. Shulamit Levenberg, a senior lecturer and researcher at the Biomedical Engineering Faculty at the Technion - Israel Institute of Technology, developed a method of creating muscle tissue that the body will not reject after implantation. Dr. Levenberg was chosen by ‘Scientific American’ magazine as one of the 50 leading scientists in the world.
Behind the microscope:
“My doctoral thesis focused on the subject of communication between cells: how cells ‘talk’ to one another and how intra-cellular signals are passed. While working on my thesis, I read about tissue engineering, and I was fascinated. Here was an opportunity to learn how cells reorganize and communicate in a living organism. After completing my thesis, I joined Professor Robert Langer, one of the pioneers of tissue engineering at MIT as a PhD researcher. My research evolved into practical implementation – we went from studying tissues to creating tissues for use in medicine.

Dr. Shulamit Levenberg (Photo: Yanai Yechiel)
“One of the problems with engineered tissue is rejection by the recipient. The process of penetrating blood vessels into the transplanted tissue is slow and the tissue might die from the lack of blood supply. For the last couple of years I’ve been working on creating tissues that can generate their own blood vessels to encourage smooth absorption.
“The first stage of my work at MIT was on muscular tissue. We succeeded in creating muscular tissue from fetal stem cells. We created biodegradable ‘scaffolding’ with a sponge-like texture and plant stem cells in the holes of the sponge. There they reproduce and form live tissue. Eventually, the scaffolding disintegrates and the newly formed tissue blends completely with the living organ into which it was transplanted. We tested successfully with animals and we proved that our method improves the absorption of implants."
‘Scientific American’ is recognized as the most prestigious scientific publication and since its inception in 1845 it has published articles by more than 100 Nobel Prize laureates. John Rennie, the editor-in-chief writes: “Our publication chose the individuals or organizations that promote science and technology and lay the groundwork for a better future.”
“I am motivated to continue my work and to further our ability to create muscular tissues for implanting and for treating diseases such as muscular atrophy,” said Dr. Levenberg.
Mending 'broken' hearts
Professor Lior Gepstein, Head of the Cardiovascular Research Laboratory in the Faculty of Medicine at the Technion - Israel Institute of Technology and a lecturer in the Physiology Department, received the American College of Cardiology's Zipes Award for his development of heart cells and pacemakers from stem cells.
Behind the microscope:
“Congestive heart failure is the main cause for hospitalization; more so than all the cases of cancer put together. Fifty percent of patients die from heart failure within 5 years of diagnosis. In cases of severe heart disease, the only available solution is a heart transplant. During the last few years, a new concept of treating heart disease is being developed whereby the damaged tissue is replaced by new tissue that has been produced from embryonic stem cells. This is what I am working on.
“About seven years ago, we succeeded in creating mature stem cells from embryonic stem cells. We were the first in the world to do that. We realized that these cells had the make up of young heart cells; with the same electrical activity and cardiac rhythms. We were very pleased – if these cells look and sound like heart cells, then they probably are.

Professor Lior Gepstein (Photo: Yanai Yechiel)
“Subsequently, we proved that these cells act in unison - a miniature heart of sorts - including an area that functions as a pacemaker. We tested the cells by placing them next to a rat’s heart cells: The two tissues' electric activity was synchronized within just a couple of hours. The next stage of the research, which has not been published yet, consisted of implanting the human heart cells we created into the heart of a rat which has congestive heart failure. We saw that the implanted cells integrated into the heart and improved its cardiac activity.
“I'm also working on developing a pacemaker that will replace the artificial ones currently used. We plan on developing the ability to create a biological version which will be implanted into the patient's body using a catheter. We tested this idea on pigs with abnormally slow heart rate and discovered that the injected cells improved the heart rate, functioning as biological pacemakers.
"Although we have had impressive results, we are still a far way away from using this technique on humans. Even so, I believe that we will be seeing experimental treatment with patients in about 10 years time".
The Zipes Award granted by the American College of Cardiology is known as a most prestigious award in its field. “Professor Gepstein is a brilliant research doctor. His scientific achievements in mapping the electric activity of the heart and in stem cell research are of the highest standard for which he deserves this award,” the award committee wrote.










