
Polina Perlman
Israel's hospital tragedy
Op-ed: Med student offers grim view on deteriorating state of Israel's hospitals
Some will refer to it as a post-traumatic state. I will never forget the night I stayed with the young resident-on-duty at the hospital. Only four months into his residency and a moment after completing his internship, he remained in charge of a ward holding 40 patients (and that's before admitting more patients from the emergency room overnight). Most of them had all sorts of illnesses, and a longer list of medications they were on.
While running around the rooms, receiving new patients, and writing new prescriptions, the relatives of an elderly man suffering from dementia arrived at the hospital. The fact that they missed the timeslot allowed for talks with the doctors by four hours at least was of no interest to them. "We demand to speak with the head of the department!" the man's devoted son said. He proceeded to insult the resident, me, and an innocent nurse who attempted to intervene. Eventually he agreed to return the next day.
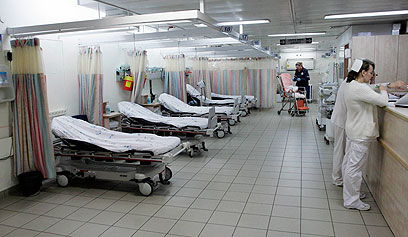
Israeli hospitals face crisis (Photo: Eliad Levy)
Doctors may work eight-hour shifts in some Western countries, with every shift comprising both specialists and residents. We can assume that in an enlightened state, an emotional relative would never treat a doctor this way, regardless of how young or junior-ranked he was. Yet this isn't the case in Israel.
Here, the system is premised on residents, who serve as both the building blocks and the fuel. Today, they are also one of the most exploited sectors within our economy. They are being trampled by the Treasury, by the Health Ministry, and certainly by the patients and their relatives; too tired and busy to complain, they merely count yet another week and another shift to the end of their residency.
A shift constitutes a full day of work, which also spills into two other days. Two days of work where you are in charge of an entire ward as the only doctor there. The senior doctor, who is on duty that evening, can offer his help by phone at times of trouble, but this resource is strictly limited. One cannot blame such doctors, as the shocking pay slip at the hospital prompts them to moonlight elsewhere in order to make a dignified living.
Vicious cycle
And so, the resident-on-duty remains alone as he receives new patients, examines them, and decides on the treatment. On occasion, he can consult with a more senior resident in another ward. If he's "lucky," he also has a young med student by his side. I have no idea how these residents have the energy to welcome and teach the students assigned to them.But how come this system continues to work? How is it that people are not hitting the streets in protest or doing something else? This reality is worrying because it's a slippery slope. "once upon a time, people would wait three weeks for an appointment, yet today it's at least two-and-a-half months," a senior secretary at a clinic in one of Israel's largest hospitals says. "That's how it is. Those who have money acquire private services, and those who don't have money wait."
The shortage of openings or attractive rewards for vital professions has turned into a serious, incurable disease. It's not as though we don't have enough doctors, or as though they are moving to countries that offer greater financial rewards; not en masse at least, for the time being. It is the public system that pushes them to the private sector at the end of their residency instead of trying to encourage them to stay in the public sector via improved terms.
This is a vicious, ongoing and mostly deplorable cycle.
Is the state of Israel's healthcare system really that terrible? An Australian med student who considers – God knows why – doing his residency in Israel asked me. It's even worse than you expect, I was thinking. The students at the various wards, like me, play the role of extras, or at most a secondary role that has only a few lines. While these students are equipped with a robe, stethoscope and a serious glare, they in fact lack any decision-making responsibility.
Yet as extras, we have the rare and transient ability to look at reality through a wider prism. Maybe that's why reality seems so bleak.
Polina Perlman, a 6th year med student at Tel Aviv University, is a Ynet news producer
- Follow Ynetnews on Facebook










