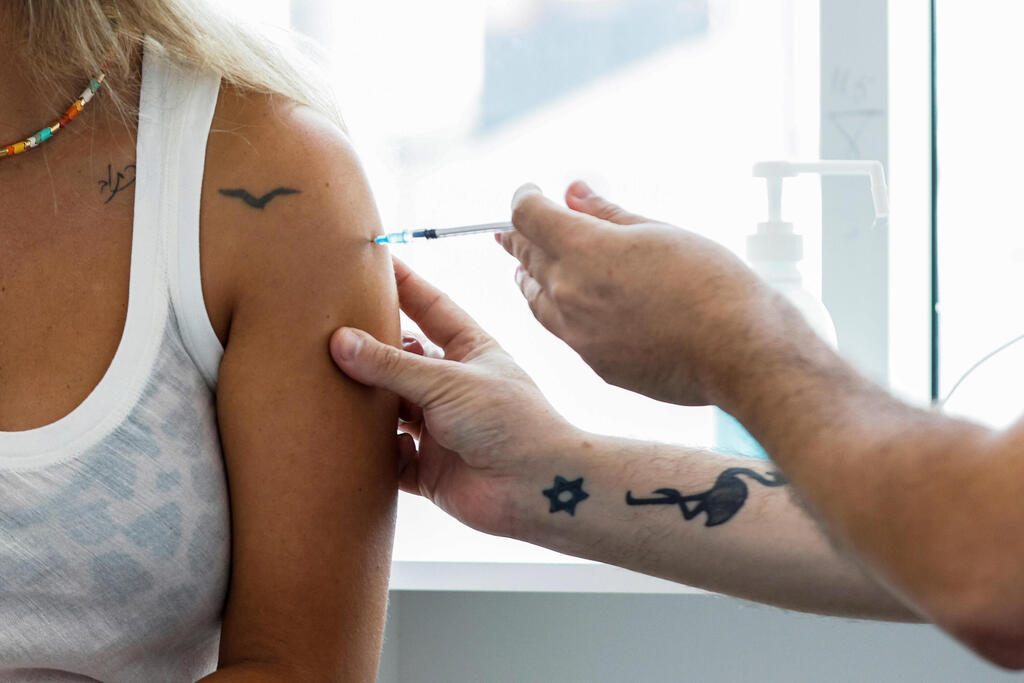
It was the biggest threat to humanity in recent years: three and a half years after the outbreak of the COVID-19 pandemic, which claimed the lives of approximately 6.87 million people, the World Health Organization declared that COVID-19 is no longer considered a medical emergency. Has the pandemic really passed, and is vaccination still necessary?
Other stories:
Global death rates dropped from over a hundred thousand per week in January 2021 to slightly over 3,500 deaths by the end of April this year. The explanation can be attributed, among other things, to the successful development of vaccines against the COVID virus, which aided in preventing severe illness, new viral strains like the Omicron variant, which caused milder symptoms among the majority of infected individuals, and, apparently, widespread exposure to the virus causing a certain level of partial herd immunity.
COVID-19 was one of the world's most extensive pandemics. Nearly 690 million people out of a population of 8 billion worldwide were infected with the virus. The pandemic led to lockdowns across the globe, a severe hit to the global economy, whose effects are still being felt today, and devastating impacts on the mental health of children, youth, and adults due to the lockdowns. The virus is still being researched for its destructive influences on physical health.
Vaccine technology improved
Despite the extensive devastation wrought by the pandemic, it has also spurred unprecedented advancements in the medical field. For instance, one major result of the pandemic has been increased awareness of the importance of vaccinations.
Despite vocal opposition to vaccine policy, and the spread of lies and severe verbal abuse directed toward vaccination program advocates, the initial response to the development of vaccines was massive, and vaccination campaigns worldwide have indeed saved lives.
Vaccination's success can be attributed to the breakthrough technology of mRNA, which led to not just highly effective vaccines but also the ability to create new vaccines within just a few weeks — a process that previously would have taken years of development and production.
This breakthrough technology has led to the development of new and highly important vaccines expected to be introduced in the near future, including against the deadly CMV virus in pregnant women, the EBV virus responsible for glandular fever and cancer, the RSV virus that causes severe lung inflammation, and the herpes virus, as well as metabolic diseases and different types of cancer.
Furthermore, as a result of the pandemic, there have been significant advances in telemedicine. Health organizations and medical clinics around the world have made strides to use remote medicine has been critically accelerated by the pandemic.
This has enabled patients to choose whether to visit a doctor in person or engage in a video call to discuss their examination results, and a variety of new remote testing devices have been developed, such as the Israeli-designed "Tyto" device that is already in use by many patients, allowing for comprehensive medical exams performed from home. Also developed is a home-based ultrasound for pregnant women, and many more diagnostic devices and procedures are expected to roll out in coming years, transforming the field of medicine.
Many still suffer from severe symptoms
COVID has also caused significant long-term damage in addition to technological advances in medicine. Alongside the incomprehensible number of deaths, and the many patients who are left with severe disabilities, the virus has also led to a new phenomenon that is still being researched - the long COVID syndrome. Increasingly, patients who have been infected with COVID-19 are showing severe symptoms long after recovery, and many continue to suffer from chronic symptoms.
According to a recent study published in the Journal of the Royal Society of Medicine, approximately 60% of long COVID patients experience internal organ damage even a year after infection, even if they only had mild symptoms during the initial infection.
Long COVID is a condition in which infected individuals continue to experience symptoms or develop new symptoms after recovery from the coronavirus. Long COVID symptoms can be wide-ranging and include fatigue, shortness of breath, chest pain, joint pain, headaches, brain fog, sleep difficulties, depression, or anxiety.
Out of 536 patients, 331 (62%) were identified with organ damage six months after initial diagnosis. These patients underwent a follow-up MRI scan six months later at the University of Oxford for all their body organs. The findings confirmed that 29% of COVID-19 patients had internal organ damage, with prolonged symptoms and impaired function, half a year and a year after infection. Fifty-nine percent of long COVID patients suffered from damage to a single organ one year after initial diagnosis.
The researchers also reported that some patients experienced symptom improvement from the sixth to the twelfth month after infection: extreme shortness of breath decreased from 38% to 30% and cognitive function impairment decreased from 48% to 38%. Also, the quality of life reported by 57% of patients decreased to 45% of patients who reported a decline in quality of life a year after infection.
Long Covid - a laundry list of symptoms
"Long COVID" is the term given to the condition where symptoms last for more than 12 weeks after being infected with COVID-19. This worrying phenomenon has led to hundreds of millions of chronic patients still suffering from the devastating effects of the virus, including children and adolescents.
Medical reports from around the world describe not only physical ailments, such as shortness of breath and a significant increase in fatigue, but also high rates of mental illness among children, including depression, eating disorders, and anxiety. Some of this may be attributed to prolonged lockdowns, but according to estimates, the virus itself may also be responsible for the widespread illness.
Some symptoms may disappear and then return, while others do not appear until the end of the illness or even after recovery. Among the symptoms reported by COVID-19 survivors are coughing, shortness of breath, fatigue, muscle pains, memory problems, anxiety, depression, rashes, and diarrhea.
There have also been reports of worsened conditions in other diseases such as diabetes and inflammatory bowel diseases (Crohn's and colitis), as well as rare but serious cases of cardiac arrests, strokes, deep vein thrombosis, heart failure, and cardiac disorders.
The diagnosis of "Long COVID" is based on clinical examination by a doctor, patient complaints, and, of course, a positive COVID-19 test. Those suffering from chronic symptoms and not diagnosed with COVID-19 will likely need a serological blood test to prove that their body has antibodies against the virus.
It is still unclear what causes Long COVID, but the prevailing belief is that the disease is caused by inflammatory processes that occur in response to the COVID-19 virus, including the "cytokine storm". These processes cause widespread damage to the body and blood vessels. Cytokines, tiny proteins secreted by white blood cells, are not normally produced by the body but are activated when a foreign agent enters the body.
The severity of Long COVID varies depending on the complexity of the disease in different patients. Experts recommend that COVID-19 survivors remain under constant medical follow-up after recovery due to the risk of thrombosis in the brain, lungs, heart, and other organs in response to the inflammatory process. For this reason, many patients who were hospitalized in critical condition and discharged still continue anti-clotting therapy, such as aspirin.
"Some symptoms may disappear and then return, while others do not appear until the end of the illness or even after recovery. Among the symptoms reported by COVID-19 survivors are coughing, shortness of breath, fatigue, muscle pains, memory problems, anxiety, depression, rashes, and diarrhea. Rare but serious cases include cardiac arrests, strokes, deep vein thrombosis, heart failure, and cardiac disorders"
The recovery of those suffering from Long COVID is carried out according to the systemic damage. Patients who have suffered lung damage will require close follow-up by pulmonary physicians and undergo pulmonary physiotherapy to improve lung function in conjunction with graded physical activity.
Patients suffering from chronic pain or fatigue will need continued follow-up at a fatigue clinic (similar to patients suffering from chronic fatigue syndrome). Since there is no specific treatment in such cases, recovery is based on physical activity, and in some cases may include hydrotherapy and treatment with anti-depressants.
Patients suffering from psychiatric disorders, including depression and anxiety, will continue to require appropriate psychiatric consultation. Recently, there have also been increasing reports of various neurological complaints, including neuromuscular disorders and weakness. These patients will need to continue neurological follow-up, which may include laboratory tests, EMG tests, MRI scans, and the integration of appropriate drug treatments with physiotherapy and physical activity.
This elusive virus is here to stay
The World Health Organization still does not know the origin of the virus causing COVID-19. In the media and the U.S. healthcare system, there is debate about the reason for the outbreak of COVID-19.
Some American agencies believe that the virus naturally spread from animals to humans in a Wuhan food market. Other agencies estimate that the pandemic was caused by a leak in the virology lab in Wuhan. This theory was considered a conspiracy theory during the peak of the global pandemic.
A few months ago, President Joe Biden signed a law requiring the American intelligence community to declassify materials related to the investigation of the connection between the coronavirus outbreak and the virology lab in Wuhan, China.
What is clear is that regardless of the origin of the COVID-19 virus, it will be with us for many years to come. The decline in mortality rates announced by the World Health Organization may indicate that the world is no longer in a state of medical emergency, but these numbers do not predict the future.
The partial vaccination of the population is susceptible to collapse at any moment because it is known that the levels of resistance generated as a result of exposure to the virus "last only half a year." Most of the population is no longer vaccinated against COVID, and the virus itself is known to create new strains at an alarming rate, one of which could become lethal at any moment.
Therefore, COVID-19 is still with us, apparently forever. The only way to deal with it, and with other viruses that we have seen and that we will see, is through vaccination. After hundreds of millions have been vaccinated worldwide, it is clear that the many myths spread by anti-vaxxers are false. Vaccines are safe, there is ample information about them, their safety is high, their efficacy against severe illness and death, and perhaps even against long COVID, is clear.
Most of the world's population, including Israelis, did not take precautions against the Omicron strain. The last vaccine they received was over a year ago, so they are not vaccinated. This worrying situation may easily lead to another wave of illness, in the same way that this virus is capable of breaking out again at any moment without prior notice.