Google Maps leads me up the cobblestone streets of the financial district, through steam geysers coming emanating from the sewers. I can make out my destination: another nondescript Manhattan skyscraper.
More stories:
I make eye contact with the security guard, but quickly look away. With nothing hinting at a clinic, I finally relent and, in a whisper, ask the guard how to get to Dr. Brooks' clinic. Without batting an eyelid, he yells: "Ketamine, tenth floor!" and gets back to whatever he was doing. People are coming and going. No one cares. This is America.
The clinic itself looks like the office of an old-fashioned law firm. Nothing here would give away that on the other side of the wall, in private cells, people are tripping right now. The reception space is designed like a colorful play area with plastic ornaments and toffee candies scattered about. Looking around the lobby, it’s easy to understand the choice of location: beautiful, young people, some evidently coming directly from a long day’s work on Wall Street, others on their way away for the weekend, donning hiking boots and carrying Mochila bags.
In cheery American, the receptionist asks me to fill out the medical forms. Tony Braxton's “He Wasn't Man Enough for Me” is playing in the background. She quickly returns to her post to serve a young man trying to set a date for another Ketamine session. "How are you today?" she asks enthusiastically. He hesitates. This should be the only place in America where you can answer "total shit" without anyone getting upset, but American protocol is too hard to overcome. The disparity between the receptionist’s enthusiastic, service-oriented tone and what actually goes on here, is just too hard to fathom.
Here – like the other Ketamine clinics sprouting up in the city like magic mushrooms after the rain – they try to convey normalcy. The patients here are "customers", not patients. Just as you might go for a day to the spa to have your body pampered, you can come to this spa to have your brain pampered. After all, when was the last time you detached yourself from your phone and spent 90 minutes staring at the ceiling, pondering life?
Ignoring the needle stuck in your vein for a moment, it sounds rather tempting. These clinics’ websites showcasing a plethora of stock photos of models, look as if they’re selling toothpaste or feminine hygiene products. If you weren’t depressed when you came in, it’d definitely put you in the mood. The treatments on offer target people suffering from depression, anxiety, PTSD (post-traumatic stress disorder), neuropathic pain and addictions. They’re also aimed at high-tech workers who’ve lost their jobs, as well as "normal" people on a quest for meaning or after a supervised trip during which they can delve deep through their own chains of consciousness.
"The full treatment recommended by doctors includes at least six sessions over a two-month period, and soars to $4500 and upwards of $5200. Being in America, you get what you pay for: In high-end clinics like Nushama, they offer a pampering trip experience in rooms with zero-gravity chairs that look like post-modern art galleries."
All this normalization is compromised as I walk down a corridor for my first conversation with the psychiatrist overseeing my session and I see another fury stuffed sloth doll. I remember seeing one at the entrance. It’s a cute gimmick but, opening the door, I wasn’t expecting a sloth temple. God knows why I didn’t leave right there and then.
It turns out that Dr. Brooks’ happy customers know quite how fond Dr. Brooks is of the tropical mammal and they bring him hundreds of them as souvenirs from all over the world as gifts of appreciation. He claims that 70% of his patients report a dramatic improvement in their lives. Over the years, he’s performed 60,000 Ketamine infusions to over 4000 patients, accounting for the sloth installation in front of me.
Ketamine and Botox
And that’s just one clinic. The Ketamine clinic scene has been buzzing for the past two years, especially in liberal, prosperous New York, a city happy to embrace innovation. In the not-so-distant past, there was no more than a handful of doctors providing Ketamine treatment, primarily in clinical settings. Now, hundreds of these businesses with varying degrees of pretentiousness, can be found across the length and breadth of the United States, offering intravenous Ketamine infusions at prices ranging from $525 to $1950 for a single session. The full treatment recommended by doctors includes at least six sessions over a two-month period, and soars to $4500 and upwards of $5200.
Being in America, you get what you pay for: In high-end clinics like Nushama, they offer a pampering trip experience in rooms with zero-gravity chairs that look like post-modern art galleries. After the session, you can spend time in the chill-out lounge with unlimited snacks and tea extracts, while browsing through “How to Change Your Mind” by Michael Pollan - widely regarded as the man who brought the psychedelic revolution into the mainstream.
Nushama’s competitor, Field Trip, which recently went public on Nasdaq at a valuation of $328 million, also offers Ketamine injections in clinics enveloped by verdant gardens that resemble clandestine ski resorts. And then there’s Trifecta which offers spa, facials and massages while you’re tripping, as well as Botox and fillers, hair removal, colonoscopies etc. Their motto is "facial, body care and brain therapy - all in one place."
Way on the other end of the scale are companies such as Mindbloom that try to keep costs down. They let you take a Ketamine pill home and offer guidance over Zoom, or the clinic that we chose – considered a pioneer in the field – but felt more like a medical center than a spa.
The nurses and doctors were friendly but, unlike in more upscale clinics, here they hold a minimalist approach and are very much opposed to all the extras. They also don’t believe in guided sessions. Patients can do their “integration” (post-trip processing) with their own personal psychologists rather than in the clinic itself.
Dr. Brooks is keen to explain that this is not to keep costs down, but rather because he believes that the guidance using visual means or music interferes with the physiological process it generates in the body, and can even be dangerous. He further believes that you don’t have to have a psychedelic experience to be cured with Ketamine:
"The out-of-body experience, euphoria and psychedelic experiences are just superfluous side effects. The benefits of Ketamine actually begin only after the infusion is over. The trip isn’t the goal. Ketamine’s role is to increase the size of the dendrites (nerve cell inputs) and the synapses (meeting area between the neuron and target cell) in the brain. It restores communication between neurons in the mood center, so you don’t have to have a hallucinatory experience to get results. It can, actually, be very dangerous to push people into dissociative experiences or into flashbacks."
Conversely, clinical psychologist, Dr. Itay Kohane, who also treats patients with Ketamine, believes the very opposite: “Your environment has immense meaning. It’s about your mindset.”
He preps me for my session. "I strongly believe in therapy with a therapist present: our treatment incorporates appropriate preparation, taking Ketamine in the presence of a therapist, and post-treatment integration sessions. I’m not a fan of the model of going to a clinic that just provides the substance. The experience itself isn’t always rational, and it can take time to integrate - sometimes up to two weeks after each Ketamine treatment. Patients don’t always know what to do with what they experience with Ketamine. This is what the therapist is there for.
“I often see it with patients who’ve had treatments in the non-medical model. They come to me for a corrective experience with appropriate preparation. The benefits are not immediately clear. It’s like the delayed pain you get after a fall. It’s not a miracle pill that fixes everything. You need to understand what you’re going through. If a patient wants to work on their relationship with their parents, for example, they may feel like a child during the experience. They won’t understand why they’re suddenly so bad-tempered or are acting childishly. It’s often somewhat veiled. Ketamine neutralizes a part of the brain that allows you to be open to more options.
Because it’s originally an anesthetic, people can experience death and rebirth. It’s a positive thing. It has enormous potential for good and we’re trying to make it accessible not only to the rich. Like everything, there’s also potential for bad things. The industry around it has become a money machine. I’m less into that.”
Doctors and pharmacists in the field have disagreed among themselves from the very moment they started using Ketamine for mental health treatment. These disagreements involve almost every aspect of Ketamine consumption: the type of treatment, accompanying process, ideal dosage and even what kind of music - if at all - should be playing in the background.
"Ten minutes into the session and I’m still staring at the flower in front of me, suspecting the drug isn’t working on me. Then, I suddenly started feeling the anesthetic – first in my mouth, then in the rest of my face. My thoughts start slowing down, relaxing and a weight falls over my body. I glide my hand over my face and can't figure out who's running this thing"
In the absence of regulation, any person or business is free to invent their own rules. They all operate legally but, in reality, the Food and Drug Administration (FDA) has never approved the use of Ketamine for mental health treatment, but only as a sedative.
One particular version of Ketamine, Esketamine (also known as S-Ketamine), prescribed as a nasal spray to treat chronic depression, has been FDA-approved. The FDA, however, doesn’t regard these medications as identical. So, the use of Ketamine in various clinics is classified as “off label” – a drug used not for its original purpose. When defined as such, FDA representatives cannot supervise it or create any kind of order in this crazy market.
All these clinics currently operate in a kind of grey area and do more or less whatever they want - mainly whatever’s good for business. “We don’t believe the state has to interfere with everything,” says Dr. Brooks. “Who’s to say it’s good that government officials should decide? We’re the experts and we decide what’s right. We employ all the safety rules of a regular clinic.”
Dr. Kohane adds that in Israel, unlike in the United States where the field has been severely compromised, there are many more hurdles preventing use. “But there’s something good about the fact that it hasn’t become commercialized and materialistic. Ketamine isn’t right for everyone. It’s important to explain to people with self-control issues or people who want to try it because it sounds cool right now, that Ketamine can have side effects.
Some might say that Ketamine treatment is equivalent to 30 years of regular therapy, but it's not that simple. Ketamine can help with some issues, but you don't have to push it, and you can definitely treat it without it."
Treatment in Israel is approved and was even included in the 2020 “health basket.” In the meantime, however, only 14 medical centers in the country provide the treatment, and appointments are limited. Israeli HMOs (kupot holim) are in no rush to approve treatment and many psychiatrists have never heard of it – so it’s not easily accessible. Here in New York, on the other hand, it's freely available to anyone willing to pay.
In the “screening” telephone conversation prior to my treatment, the nurse explains the procedure and tries to reduce my expectations. “I don’t know what kind of experience you’ll have. I can’t promise anything. People often come in here and want to delve deep, overcome hurdles and change the way they see life. That sometimes happens, but there’s a 50% chance that it won’t. Definitely not your first time. It takes at least three sessions to feel any kind of change. We recommend coming back for a “booster” every six months to reinforce the effect.”
What if I feel I want it every day? Can I become addicted to the good feeling?
“Generally, there’s no problem of addiction. There’s a difference between being addicted to a good feeling and a physical addiction to the drug. It very much depends on the person and their proclivity to addiction. To avert this, we reduce the dosage. Dosage is an art. We take extra care."
I open up and tell her about my most recent experience with psychedelics and how awful it felt. I tell her how I experienced death and suddenly realized how much self-loathing I was harboring deep within my body. The other end of the phone went quiet. “So would you like to come in this Wednesday or next?”
Rolling laughter in the next room
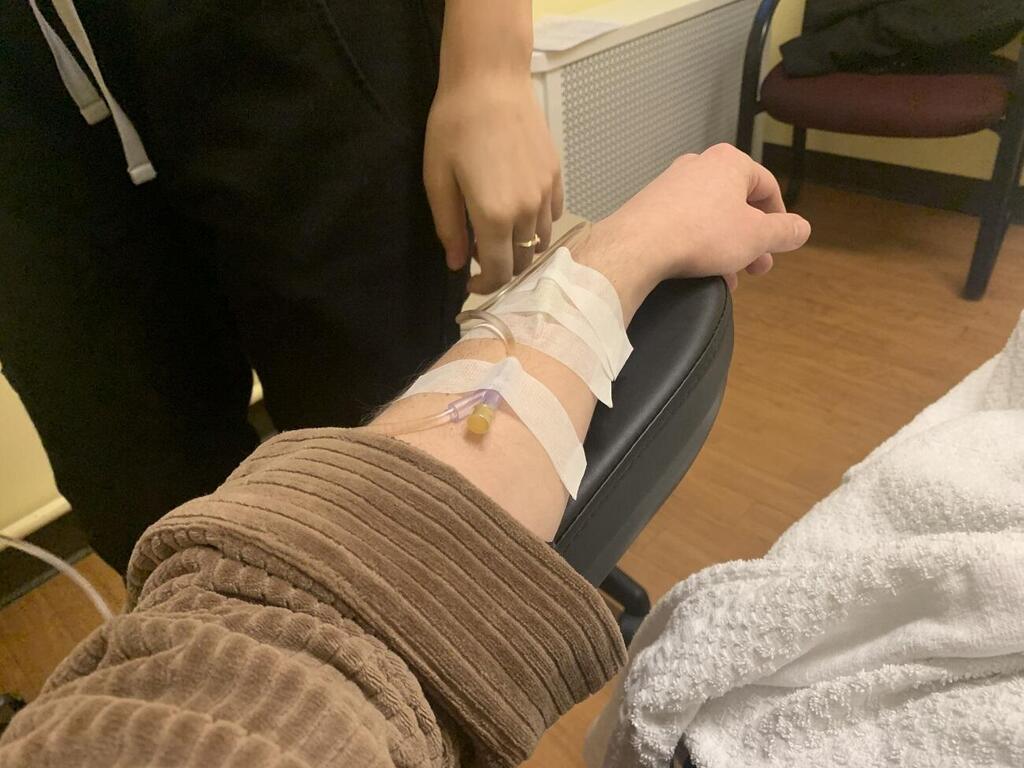
On treatment day, I was asked to fast for at least two hours to prevent nausea. After a remarkably productive preparatory conversation with the doctor at the sloth office/temple, in which we delved deep into my life, my fears (talkbacks) and concerns, the lovely nurse led me to the minimalist IV room.
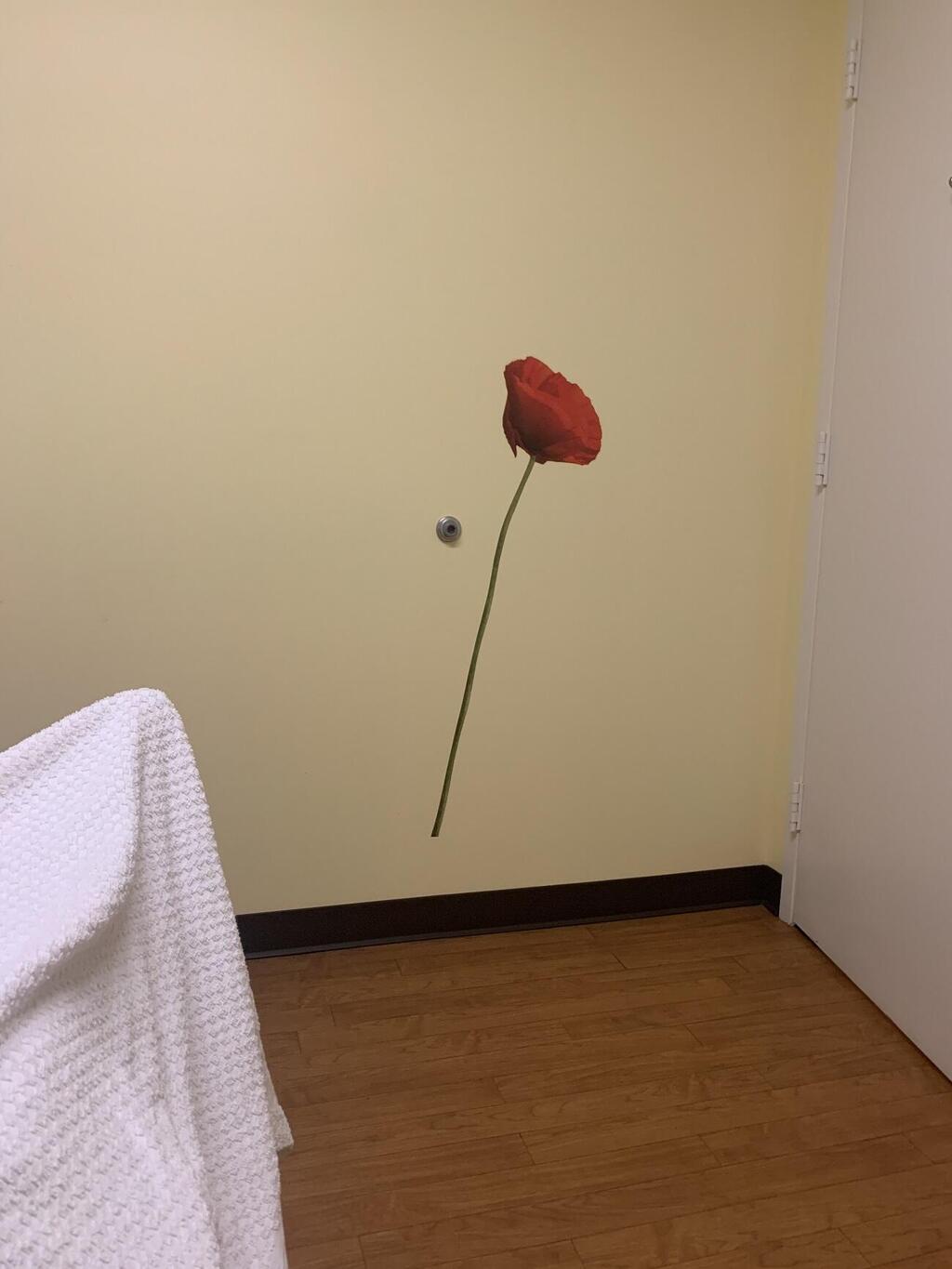
In the center of the room is a dentist's chair. On the wall, there’s a lone drawing of an opium poppy that later transformed into a 3D image in my brain. The nurse covered me with a blanket, asked what kind of lighting I wanted and gave me a blindfold and Bluetooth headphones in case I wanted to listen to some music. I recalled the preparatory conversation with Dr. Kohane, who stressed the importance of music during a trip, claiming that the music is more important than the therapist. He recommended that the music should have no lyrics, or at least be in a language I don't understand. The music should, start out tranquil and become more intense, forcefully melancholic.
I started getting nervous. Where would I find something meeting all these criteria? I turn to the gods of Spotify, which in a matter of seconds presents hundreds, if not thousands. of "Ketamine playlists." The nurse sees me trying to navigate the vast selection: "Go for Bob Marley. Trust me."
Ten minutes into the session and I’m still staring at the flower in front of me, suspecting the drug isn’t working on me. Then, I suddenly started feeling the anesthetic – first in my mouth, then in the rest of my face. My thoughts start slowing down, relaxing and a weight falls over my body. I glide my hand over my face and can't figure out who's running this thing. My mind was hovering over my body, and suddenly there’s no connection between the person inside and this pile of meat, tendons and flesh. My body appeared muscular in a distorted kind of way, like the tree trunk of a leafy tree creaking with every tiny movement.
I gaze at the palm of my hand, turning it right and then left, like some kind of heavenly puppeteer, and can just about write down a few words for the article: "body", "muscles", "flesh", "veins", "heavy movement", "David Dvir", "Martha Graham", "Pinocchio wooden hands", "hand like a robot", "Elon Musk-like arm", "ET Phone Home."
I suddenly feel heart palpitations and difficulty breathing. I remember what Dr. Brooks said about them making up the rules for themselves here. I want my mom. I want my dad. Then the paranoia sets in. What happens if I die here? How do you say Magen David Adom in English? Who do I trust here? I’m sweating and moving around uncomfortably. I immediately calm myself down – all will pass. You know what I mean. And then I let myself enjoy the moment.
The highest transcendence is in the seconds in which the music syncs perfectly with your thoughts. For me, it was songs with lyrics that at that moment somehow resonated like divine insights. Since then, Spotify has been offering me this same playlist while in a fully conscious state. I’m hearing "I Feel Peaceful" and “My Heart is Open" in a freaky loop while lifting weights at the gym. It's definitely not everyday music. Oh and another thing: don't skimp on the add-free premium subscriptions. Nothing puts an end to a trip faster than an advertisement for Taylor Swift novelty items.
The nurse comes into the room every 15 minutes to check that everything is OK. On each visit, she looks stranger and stranger. On her final entrance, she looked like an ostrich with a head slightly peeking above that long neck. I feel that she feels that I feel that she’s strange, which evokes its own trip. Maybe Dr. Brooks was right and these sessions should be conducted without any kind of accompaniment.
As she leaves the room, I hear the rolling laughter of someone tripping in the next room. All of a sudden, every situation seems bizarre to me. On the one hand: What the hell are we voluntarily putting in our bodies? On the other: How can anyone go through life without experiencing this thing? How many opportunities do we have in our limited time here to transcend above all the structures, boundaries, mundane and routine?
Time passes quickly and my body starts getting tired. I want to sleep. I didn’t want it to end though. I felt I was getting somewhere. Ostrich came in and told me that the infusion will be coming to an end in ten minutes. Like a junkie, I pled for more. Accustomed to this, she ignores my pleas.
After the infusion, I remained in the room for at least another two hours, like a stone block, unable to move. The nurse, who by now had reverted to being human, told me to take my time – while changing the sheets for the next patient. I got the message, but was exhausted. It was a classic, low-intensity, 90-minute mini-trip – but it hit all the spots: disassociation, paranoia, transcendence, being pissed that it’s all over soon, and finally – the desire for more and addiction. I turned off the flight mode on my phone and was bombarded with 20 unanswered e-mails and phone calls. Back to reality. The accompanying psychiatrists came into the room asking how it went. But it was almost five o’clock and she really just wanted to go home.
Reevaluate your body
The history of Ketamine could easily fill the script for a Hallmark drama series: its use began in the Vietnam War, where it proved itself in the field as a safe and effective anesthetic for painful medical procedures. It has never been considered typically psychedelic, but rather dissociative, and it’s still used regularly as a medical anesthetic. If you've recently undergone any kind of surgery, chances are you've had a taste of it, too. It is also widely used in veterinary medicine, earning it the moniker "the horse anesthetic."
Soon after Vietnam, people realized that taking Ketamine was rather fun. By the ‘90s it was a must-have clubbing drug. It's still popular as a recreational drug in some circles, some might say, mostly among disaffected teenagers who can’t afford coke. The twist in the plot was when researchers noticed that it was, within hours, effective for treating depression and mental health issues.
For over 20 years, Ketamine has been generating much enthusiasm within the psychiatric community as a quick substitute for antidepressants which can take weeks to kick in. Studies have shown that Ketamine in high doses – much higher than those taken at raves - could help patients who had been non-respondent to other treatments and had been regarded as "resistant to treatment."
Despite all this excitement, researchers still don’t know exactly how Ketamine acts on the body. The leading theory, as mentioned above, is that it causes the regrowth of synapses, and rewires the brain into a healthier and more functional state. Researchers have proven this on animals, but the process itself, its timing and consequences are still unclear and are yet to be proven.
A further reason for Ketamine captivating researchers is that it works differently from existing antidepressants. Unlike standard antidepressants that affect just one neurotransmitter (i.e. serotonin, norepinephrine, or dopamine), Ketamine acts on glutamate, the most plentiful chemical messenger in the brain.
Glutamate plays an important role in the changes undergone by synapses in response to learning and memory experiences. This is why researchers believe that such "neuroplasticity" lies at the heart of Ketamine functioning as an antidepressant.
Very little is actually known about the biology behind the mechanism of depression, it’s remission and relapse. Ketamine’s main drawback – apart from the side effects, including out-of-body experiences, addiction, bladder problems and nausea – is that it simply isn’t medication. Most patients suffering from chronic depression will eventually relapse, and the effects of even very high doses ware off within a matter of weeks or months.
I can’t vouch for other side effects, but I definitely felt the nausea. It attacked me after I finally managed to pick myself up off the clinic chair and drag myself into the subway. They say that one of the immediate effects of the treatment is a deeper understanding or our surroundings and of ourselves. I definitely felt that, but it might have been more looking into my esophagus so as not to vomit onto the woman in front of me.
If I learned anything from this story, it’s that we have no idea what people are experiencing within themselves. And now, as I sway with a shopping basket, stumbling among the lettuce at the supermarket, as the saleswoman rolls her eyes, I know that she has no idea where I was an hour ago. Don’t judge me.
In the hours immediately following the treatment, I felt challenged both physically and emotionally. It was impossible not to, once again, appreciate my own body – the same body from which I felt disconnected during the trip. The same body I hated. The same body we abuse because of our troubled psyche.
And the next morning, like nothing happened, it woke up like new – and with an inexplicable sense of peace and inner optimism. Astonishing. I survived. I love you.