With the report of another fatality in the coronavirus crisis, many of the staffers working on the frontline in Israel's hospitals are feeling a distinct sense of desperation.
At the Meir Medical Center in Kfar Saba, medical staff are treating 23 coronavirus patients - four in serious condition - in an impromptu ward that was erected at a moment's notice two weeks ago.
“It isn’t easy," admits Wafia Nasser, a nurse on the ward.
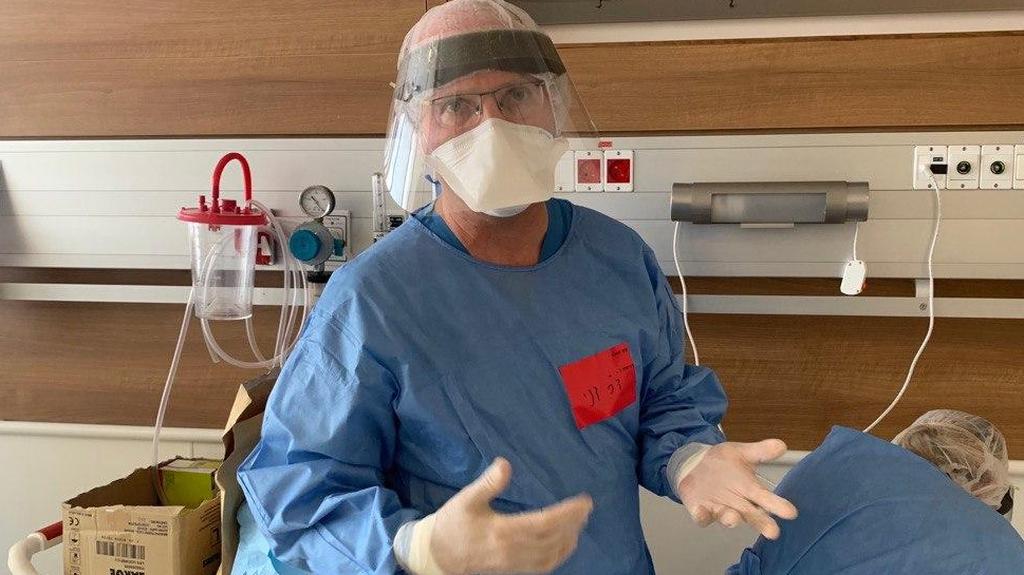
Before treating any patients, the medical team must first protect themselves. It is a slow process that usually requires assistance. The staff must don a protective suit, hair covering, disinfects their hands, put on gloves and finally add protective eye wear.
Until last Wednesday morning, most of the ward’s patients had either light or moderate symptoms. Statistically this is still the case, but now three patients have seen their conditions deteriorate.
All patients are under constant video surveillance and staff interact with them are frequently to monitor their condition. But since the patients deteriorated, ward chief Dr. Daniel King has taken it upon himself to visit the patients personally.
“This illness is changing and so is our attitude to the disease,” King, a specialist in pulmonary disease, tells the relatives of one of his patients.
"We are using certain medication that we believe is the best for the patient.”
Research into COVID-19 is happening on an ongoing basis; after doctors finish a shift and return home they often read articles and converse with colleagues both in Israel and abroad.
“One of the things we noticed and didn't read in the books,” says King, “is that patients who were put on respiratory aid appeared to be stable, only to deteriorate a few hours later. We are seeing patients immediately deteriorate after receiving respiratory aid - or they don’t [at all].”
“The fear is for the patients,” says King. “You worry what will happen to them, Right now we have to be very alert and keep a close eye on the two patients whose condition has deteriorated.”
Shortly after the ward’s director and head nurse leave the hospital for meetings, a code 222 comes from the ward - meaning a patient who was in moderate condition is showing signs of respiratory failure.
The staff, which includes two doctors and a nurse, must quickly suit up and get to the patient to perform CPR, all the while being escorted by another nurse whose job it is to make sure that the staff remains adequately protected despite the stress.
“We need to know how to perform CPR while keeping ourselves safe,” says King. “Luckily by the time we got into the room the patient had stabilized. His rate is still high, so we are keeping a close eye on him.”
Martin is a coronavirus patient who has been on the ward for three weeks, and contracted the virus during a trip to Italy.
“ i feel completely healthy,” he says, “but the virus is still there. I don’t have any symptoms, but tests show it is still there.”
“I wake up each day hoping for negative results,” he says. “I spend the days reading and listening to the news, to be honest I think this isolation is harder on my wife.”
Simha and Ahuva Yitzhaki are also patients on the ward and contracted the virus during a trip to Egypt. They expected to leave the ward soon and move to one of the hotels dedicated to coronavirus, due to their improving conditions.
“I ordered my husband and myself a room at the Dan Panorama hotel for the weekend. I hope we really do get out of the ward,” says Ahuva, who often offers mental support for those in the ward - patients and relatives alike.
When one patient began to cry after learning her son had contracted the virus, Ahuva immediately rushed to her aid.
“When I heard her cry, I jumped out of bed and asked her what happened," she says. "When she told me, I got her out of bed and we went to have tea and candy."
At present, the coronavirus ward at Meir is actually part of the Intensive Care Unit, although the hospital is considering turning its entire sixth floor into a dedicated coronavirus ward.
“The whole floor will become the coronavirus ward,” says King. “If things get worse, the entire floor will become one giant ICU. It's is better we make preparations now and things do not deteriorate than to have things deteriorate and us be ill-prepared.”
When it comes to the national situation, King prefers to keep his own counsel.
“No one knows exactly how to best deal with the situation," he says. "I can't really judge if things are being done the best way on the national level.”
He is however angry at those who fail to understand the scale of the epidemic.
“It’s infuriating that people fail to adhere to [Health Ministry] instructions," he says. "I would not know how to deal with a tsunami of critical patients.”