Can what happens in the belly directly affect the brain, even years later? A large and unusual Israeli study now offers an answer that is both troubling and encouraging: It is not weight itself that matters, but the type of fat we accumulate.
A long-term MRI study led by Professor Iris Shai of Ben-Gurion University of the Negev and Reichman University found that lower cumulative exposure to deep abdominal fat, known as visceral fat, was significantly associated with slower brain aging, better preservation of key brain structures and stronger cognitive function in late middle age. The link was found regardless of weight loss.
3 View gallery


Israeli study links deep abdominal fat, known as visceral fat, to brain aging
(Photo: Shutterstock)
The study, published in the journal “Nature Communications,” is considered the first of its kind to connect repeated brain MRI scans with cumulative exposure to visceral fat over many years, pointing to a direct link between belly fat, brain aging and cognitive function.
The study was based on advanced MRI scans of the brain and abdomen and included 533 late-middle-aged men and women who were followed for five to 16 years after taking part in four major long-term, controlled clinical nutrition trials: DIRECT, CASCADE, CENTRAL and DIRECT-PLUS. All were led by Shai, who also serves as dean of sustainability at Reichman University and is a professor at Harvard University.
During follow-up, participants underwent repeated MRI measurements to assess visceral fat and brain structures, along with cognitive testing using MoCA, a brief and widely used test that evaluates functions such as memory, attention, language and reasoning.
The fat that puts the brain at risk
The findings consistently showed that the lower the participants’ cumulative exposure to visceral fat (the deep abdominal fat surrounding internal organs), the higher their cognitive scores and the better their brain structure was preserved. This included total brain volume, gray matter, which is responsible for information processing and cognitive function, and the hippocampus, a key memory center that is especially sensitive to aging.
The study also found better preservation of the hippocampal occupancy score, a research measure sensitive to changes linked to brain aging.
 Prof. Iris ShaiPhoto: Nir Slakman
Prof. Iris ShaiPhoto: Nir SlakmanAt the same time, researchers observed a slower expansion of the brain’s ventricles, cavities that tend to widen as brain volume is lost. That process is considered a clear marker of brain atrophy, meaning a decline in brain volume caused by the loss of nerve cells and the connections between them. When accelerated, it is linked to declines in memory, concentration and reasoning.
One of the study’s central findings is the unique role of visceral fat compared with other common measures. The link between fat accumulation and brain aging was not found with superficial subcutaneous fat, the fat beneath the skin, deep subcutaneous fat or body mass index (BMI), commonly used to assess overall obesity. The finding underscores that not all types of fat affect the body and brain in the same way.
The researchers also found that a reduction in visceral fat during an 18-month dietary intervention predicted better preservation of brain structures five and 10 years later, even after accounting for weight loss and other factors. In other words, the key factor was not weight loss itself, but the reduction of deep abdominal fat.
Which fat did you lose?
That raises a central question: How can people know whether their weight loss reflects a reduction in the right kind of fat? “That is the million-dollar question,” Shai said. “Weight loss needs to be quality weight loss, not just how many kilograms you lost, but which tissue you lost: fat, muscle or less relevant types of fat.”
She said the question is especially important in the era of weight-loss injections, because some people may also lose a significant amount of muscle mass. “As of now, there are no simple blood-test markers that can identify a reduction in visceral fat, and the accurate way to assess it is through imaging,” she said. “We are working to develop markers that will make this easier and more accessible.”
Significant preventive potential
What explains the link between belly fat and brain aging? According to the study’s analyses, the answer runs through blood sugar regulation. Fasting glucose and HbA1c, a measure that reflects average blood sugar over time, were the only factors that predicted the pace of changes in brain structure. Blood lipid markers and inflammation markers did not show a similar connection.
“Blood sugar balance is the central factor linking visceral fat to brain longevity,” Shai said. “We found that it was the variable that best explained the protective effect on the brain, more than other measures we examined, such as blood lipids or inflammation.”
That means the problem is not only the amount of fat, but its metabolic effect, especially its impact on blood sugar balance, which may accelerate brain degeneration.
More broadly, the researchers point to significant preventive potential. “The brain naturally loses volume over the years, and the challenge is to slow that process,” Shai said. “Our findings show that the lower the exposure to visceral fat over a lifetime, the more we may be able to slow the decline in brain volume and better preserve brain function.”
3 View gallery
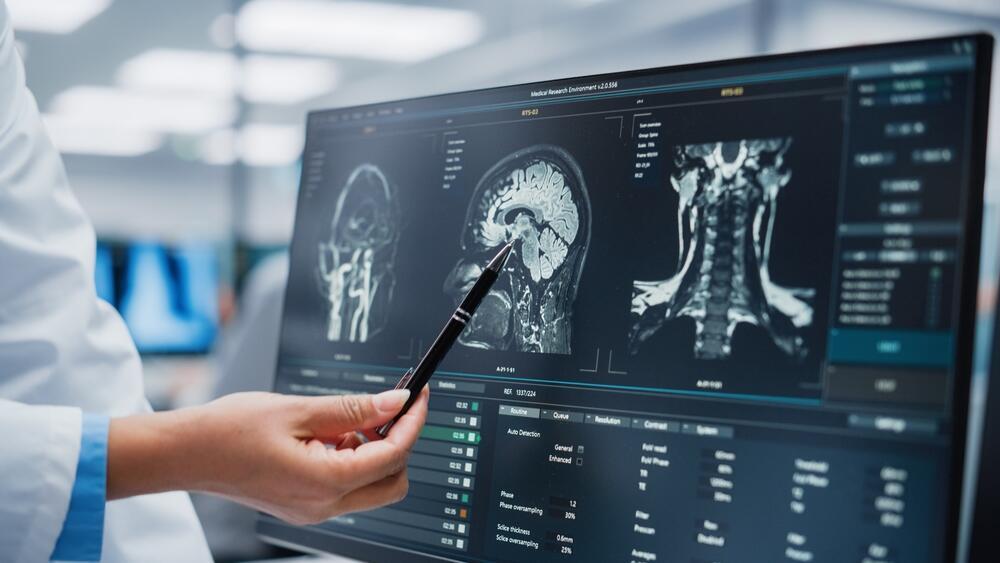

Lower visceral fat levels were linked to better preservation of brain structure
(Photo: Shutterstock)
What can be done in practice? According to the researchers, several steps specifically target visceral fat, including moderate aerobic exercise, reducing simple carbohydrates and adopting a Mediterranean diet. “We saw that this diet led to a more significant reduction in visceral fat compared with other dietary patterns,” Shai said. “It includes a substantial reduction in red meat consumption, lower carbohydrate intake and an emphasis on plant-based components such as green tea, Mankai and walnuts.”
Asked whether brain damage can be reversed, rather than merely prevented, Shai said the answer remains unclear. “At this stage, we are focusing on prevention. As for rehabilitation, that is a research direction that will need to be examined later,” she said. Still, she added, it is already clear that the mechanism is unique: “Visceral fat secretes substances with harmful effects, a process we did not see in subcutaneous fat.”
What is worth checking
The findings also challenge common assumptions about standard health measures. “BMI is no longer sufficient for assessing health or success in weight loss,” Shai said. “It does not reflect body composition and does not allow us to understand where fat is accumulating. “Waist circumference can offer a better indication of abdominal fat, but it is still imprecise. In any case, BMI is not a target and is not linked to preserving brain health.”
3 View gallery
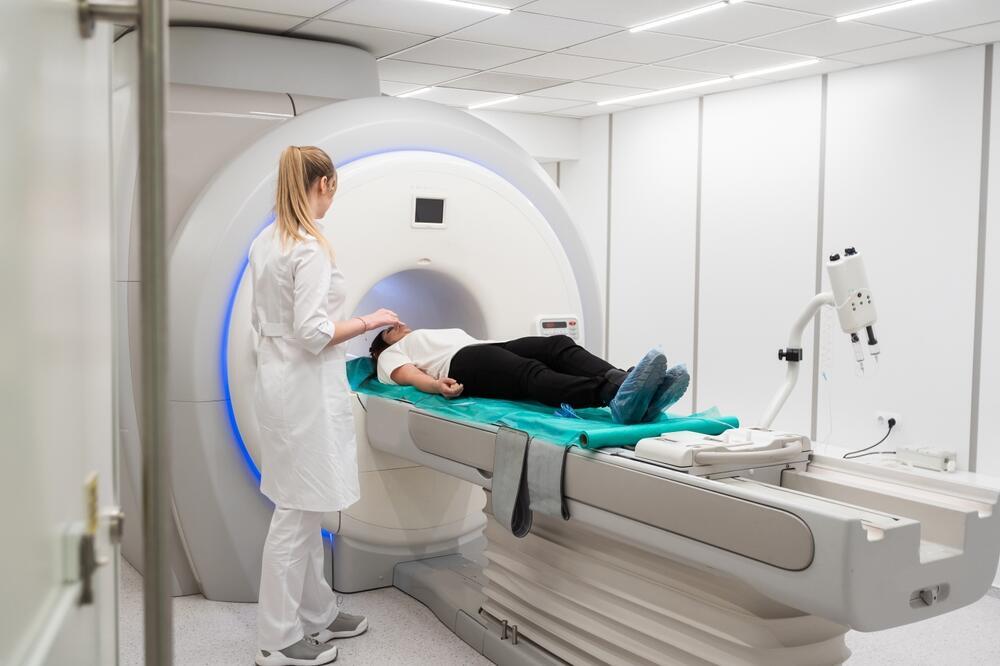

Repeated MRI scans made it possible to track changes in brain structure over the years
(Photo: Shutterstock)
Dr. Dafna Pachter, the study’s first author, added that "weight alone is not a sensitive measure of the deep metabolic changes taking place in the body. Even when weight loss is moderate, a sustained reduction in visceral fat, as measured over time, appears to help preserve brain structure and slow atrophy.”
The importance of the study lies in its scale and duration. It is the largest and longest study to date linking cumulative exposure to visceral fat with the pace of brain aging and cognitive function through MRI measurements. By combining repeated measures of abdominal fat, brain structure and cognitive function, the study makes it possible for the first time to identify a specific metabolic target, rather than general obesity, as a risk factor for brain health.
The study was conducted at Ben-Gurion University of the Negev in collaboration with researchers from Harvard, Leipzig and Tulane universities, the Nuclear Research Center Negev in Dimona, Brehita Medical Center and Soroka Medical Center, with the participation of many Israeli researchers in medicine, nutrition and neuroscience.
Shai’s research was funded by grants from the German Research Foundation (DFG) and ERA-4-Health.
First published: 23:48, 05.04.26


