Researchers at Northwestern University have reported a significant step forward in spinal cord injury research, demonstrating early signs of nerve repair in lab-grown human tissue.
The study, published in the journal Nature Biomedical Engineering, describes for the first time laboratory models that mimic human spinal cord injuries and test an experimental treatment that has previously shown promising results in animal studies.
4 View gallery
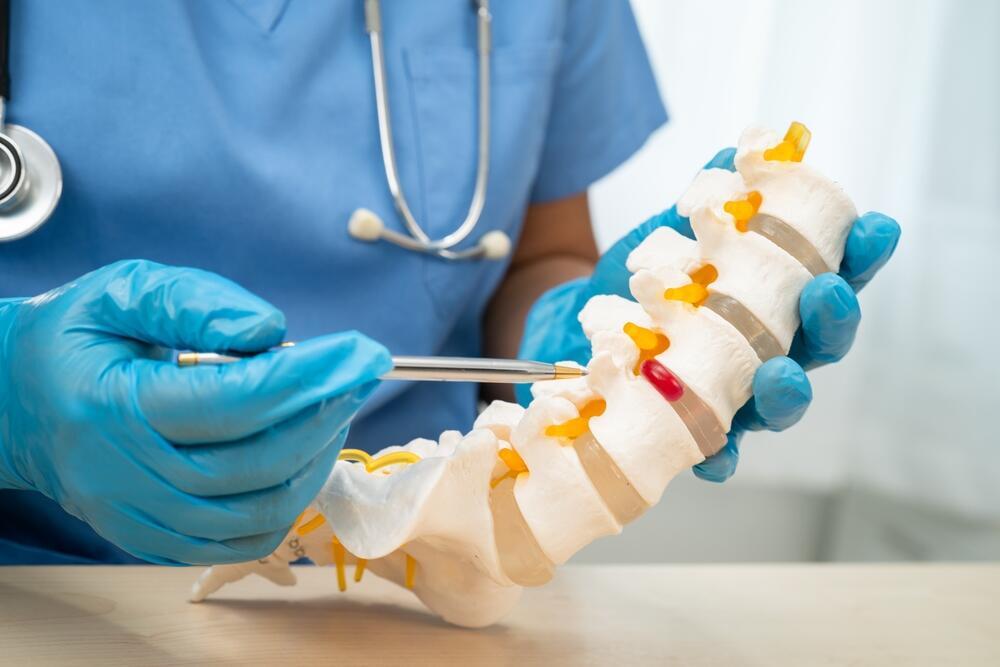

Lab-grown human spinal cord tissues were used to examine injury and repair processes
(Photo: Shutterstock)
To conduct the research, scientists developed human spinal cord organoids, tiny three-dimensional tissues grown from human stem cells that replicate key features of the spinal cord, including neurons, support cells and immune cells of the nervous system. Using these tissues, the team was able to recreate characteristic spinal cord injuries in the lab and test therapies directly on human tissue rather than relying solely on animal models.
Injuries mimicking surgery and trauma
The researchers created two types of injuries in the organoids: a sharp cut simulating surgical damage and a compression injury resembling trauma from car accidents or severe falls. In both cases, they observed immediate neuron death, an inflammatory response and the formation of scar-like tissue known as a glial scar, a well-documented process that hinders nerve fiber regrowth after spinal cord injury.
Following injury, the organoids were treated with an experimental therapy based on supramolecular structures of peptide amphiphiles, tiny molecules capable of self-assembling into dynamic structures within tissue. The researchers have referred to them as “dancing molecules” because of their motion and shape-shifting properties, which are designed to influence the environment around nerve cells and encourage repair. The same therapy previously demonstrated in mice the ability to reverse paralysis after acute, severe spinal cord injury.
According to the researchers, treated tissues showed marked changes. The glial scar-like tissue was significantly reduced, levels of inflammation-promoting factors declined and regrowth of axons and neurites, nerve projections essential for transmitting signals in the nervous system, began to emerge.
The team also incorporated microglia, the immune cells of the central nervous system, into the organoids. These cells are typically absent from such models. Their inclusion allowed the tissue to respond to injury in a way more closely resembling what occurs in an actual human spinal cord, strengthening the model’s relevance for future therapeutic testing.
The major challenge of spinal cord injuries
Dr. Itzhak Engel, head of the spinal surgery unit at Meir Medical Center, said understanding the significance of such studies requires recognizing what makes spinal cord injuries distinct from other nerve injuries.
“In spinal cord injuries, the problem is not simply a torn nerve but a complex bodily response to trauma,” Engel said. “A scar forms that blocks the passage of nerve fibers, and at the same time, the portion of the nerve beyond the injury site degenerates, a natural process that makes recovery extremely difficult.”
He noted that unlike peripheral nerves in the arms or legs, the spinal cord contains an enormous number of very long nerve fibers that travel complex, nonuniform pathways over considerable distances to reach muscles and other targets.
“Even if we imagine for a moment that no scar forms, you would still need to rebuild all those fibers in exactly the same order and connect each one to the precise target,” he said, comparing the spinal cord to a densely wired electrical cabinet. “It is not enough to replace the wires. Each one has to be reconnected to the correct outlet.”
 Dr. Itzhak EngelPhoto: Meir Medical Center
Dr. Itzhak EngelPhoto: Meir Medical CenterOver time, the scar tissue thickens and becomes a physical barrier, further limiting the ability of newly forming nerve fibers to cross the injury site. “All these factors explain why, in patients who develop paralysis after spinal cord injury, the likelihood of significant improvement is very low,” Engel said.
4 View gallery

A spinal cord injury is not a simple tear but a disruption of a complex and intricate neural network
(Photo: Shutterstock)
Most research in the field, Engel added, focuses on reducing scar formation and enabling regeneration of the cells that form nerve fibers. He noted that Israeli researchers, including a team at Tel Aviv University led by Prof. Tal Dvir, are also developing stem cell-based spinal cord implants that have shown functional recovery in animal studies and are expected to move toward initial compassionate-use trials in humans, pending regulatory approvals.
Understanding the mechanisms of injury and recovery
Prof. Samuel I. Stupp, who led the Northwestern study, emphasized the importance of testing therapies directly on human tissue.
"One of the most exciting aspects of organoids is that we can use them to test new therapies in human tissue. Stupp said, according to the TechJuice website. "Short of a clinical trial, it’s the only way you can achieve this objective."
He said the team intentionally developed two different injury models to test whether the organoids’ response to treatment would resemble findings from animal studies.
“After applying our therapy, the glial scar faded significantly to become barely detectable, and we saw neurites growing, resembling the axon regeneration we saw in animals", Stupp said. “For us, this suggests the therapy has a good chance of working in humans.”
In previous animal studies, a single injection of the therapy administered about 24 hours after severe injury helped mice regain the ability to walk within weeks. The current study did not assess functional recovery but documented structural and biological changes consistent with known processes of nerve repair.
Researchers emphasized that their aim is not to engineer an entire spinal cord in the laboratory, but to create a research platform that deepens understanding of how injury and recovery occur and to evaluate treatments more accurately and safely before advancing to human clinical trials.
The new models, they say, could accelerate the development of treatments for spinal cord injuries and may, in the future, also aid research and therapeutic advances for other central nervous system damage caused by trauma or disease.
Dr. Engel cautioned against overinterpreting the findings. “In studies, we see mice walking again, but the difference between a mouse body and a human body is enormous,” he said. “The distances are longer, the system is far more complex and the central challenge is how to ensure that new cells reach exactly the right final destination. The road from here to a cure in humans is still very long.”