Professor Ronen Leker, director of the Stroke Center at Hadassah Medical Center in Jerusalem and chairman of the Israeli Stroke Society, typically handles about 10 to 15 patients a day suspected of having a stroke. On average, about four of them are hospitalized.
Since the outbreak of Operation Roaring Lion, however, he says there has been a sharp decline in the number of people arriving at emergency rooms. “We saw the same phenomenon during the COVID pandemic,” Leker told ynet. “We fear that patients with mild strokes who could deteriorate will avoid going to the ER, and by the time they finally reach the hospital they may already be in a condition we cannot treat.”
According to data from the Israeli Stroke Society, which is part of the Israel Neurological Association, about 100,000 people in Israel arrive at hospital emergency rooms each year with suspected strokes. Of those, about 20,000 are ultimately diagnosed as stroke cases, which means an average of 274 Israelis reach emergency rooms every day with suspected strokes.
A survey by the society found that since the war began, the number of such ER visits has dropped by about 30% nationwide. In some hospitals the decline has been especially dramatic. At Hadassah, for example, between 10 and 15 people with suspected strokes typically arrive each day during normal times, whereas on one recent day, only one patient arrived. Only a few hospitals reported no change in the number of patients.
“It makes no sense that there are suddenly fewer strokes,” Leker said. “We believe people are afraid to leave their homes and come to the ER because of the war. In the first days of war there was widespread panic, and people assumed the emergency rooms were overwhelmed with war casualties, so they neglected their everyday medical problems.”
He warned that the trend could lead to a sharp increase in deaths from stroke and in the number of patients left with severe disabilities.
 Prof. Ronen Leker Hadassah Medical Center
Prof. Ronen Leker Hadassah Medical CenterNeurologists are urging the public to seek medical help immediately if symptoms appear. “I call on citizens not to hesitate, not to wait, and not to stay home,” Leker said. “Call an ambulance immediately when the first worrying signs of stroke appear. Even if you’re sent home afterward, nothing happened. The chance of suffering irreversible damage from a stroke is far higher than the chance of a missile hitting you.”
Dr. Jeremy Molad, deputy director of the neurology-stroke department at the Tel Aviv Sourasky Medical Center, said the decline in ER visits is evident. “We saw a similar trend during previous major security events, such as October 7, during the previous war with Iran and at the start of the COVID pandemic,” he said. “Typically, things stabilize after a short period as the initial fear subsides.”
 Dr. Jeremy MoladPhoto: Courtesy
Dr. Jeremy MoladPhoto: CourtesySo far, he said, there have been relatively few cases of patients with severe strokes arriving too late to receive treatments such as clot-busting medication or brain catheterization. “At the same time, we assume that many patients remain at home, mainly because their initial symptoms are not dramatic,” Molad said.
“This has two major consequences. First, some patients’ medical conditions may worsen by the time they reach the ER later, when our ability to help them is already much more limited. Second, they are not examined and do not receive treatment to prevent another stroke. In such cases, patients may not arrive now but could come weeks later in far worse condition."
“Time equals brain, that’s the number one mantra,” Leker said. “The later a patient arrives, the smaller the chance we can help. There is a clot-busting drug known as TPA, which is administered intravenously within four and a half hours from the onset of symptoms. Mechanical thrombectomy procedures can be performed up to 24 hours after symptoms begin, though only a small portion of patients qualify.
“There are situations in which the damage is already irreversible and we simply can no longer help,” he said.
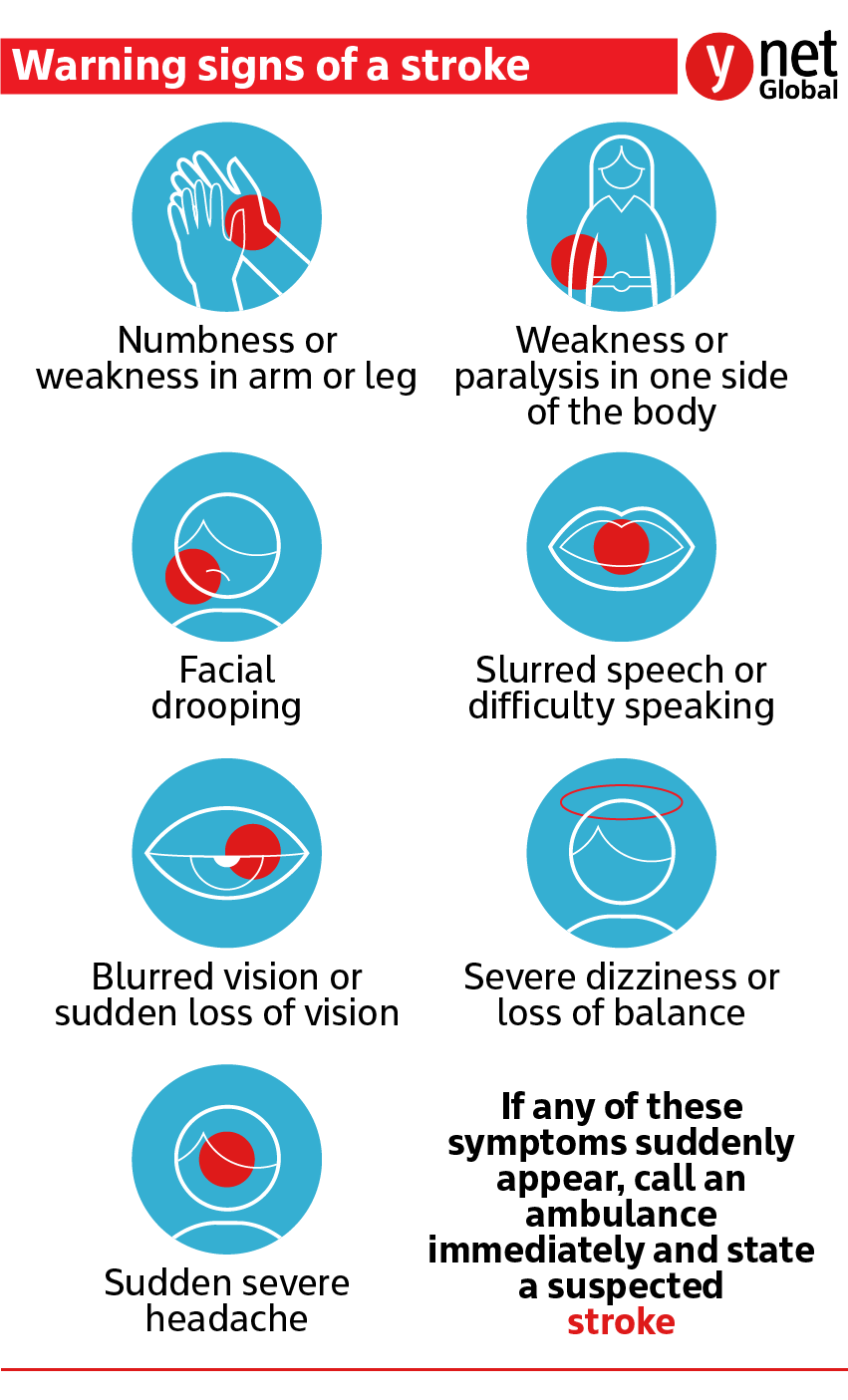
Warning signs of stroke include:
- Sudden weakness on one side of the body
- Speech difficulties or drooping of one side of the mouth
- Blurred vision or sudden vision loss, usually in one eye
- Severe dizziness accompanied by loss of balance
- Sudden confusion with difficulty understanding language.
First published: 12:38, 03.09.26