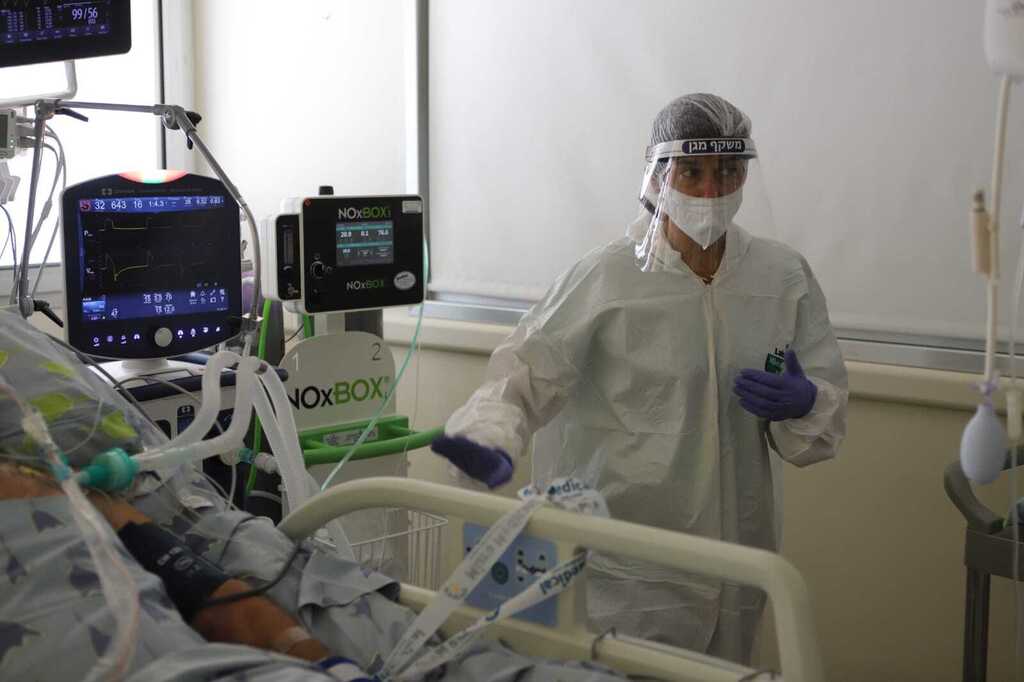
An approximate 75 percent of the medical staff and over 80 percent of the nursing staff at Tel Aviv's Sourasky Medical Center who responded to a questionnaire on their mental state amid the pandemic, reported that their struggles in the past year "left a significant mark that may affect them later in their personal and professional lives."
This statistic joins a host of reports and claims from hospital medical staff members about post-trauma and other significant emotional struggles after the pandemic year.
Between the second and third outbreaks, the hospital initiated an emotional support program for doctors and nurses in which they were instructed on how to communicate with the families of patients.
"The teams have given above and beyond in the last year and withstood every task, at all levels," explains Dr. Orly Barak, director of Sourasky's Physicians' Promotion Unit. "Many teams were transferred to the coronavirus wards even though this type of treatment was not their bread and butter," she said.
"Team members in the coronavirus wards felt they did not have knowledge about this disease and did not know how to deal with it. We did not really know what was best for this disease and the staff felt the burden and also felt that they could not give the care we are used to or want to give. It caused dissonance in terms of our perception of ourselves as therapists. "
Barak says the program was devised without any help from the Health Ministry.
"We read about it mainly in the literature, but there was no precise and orderly procedure in place. The Health Ministry says that doctors should be supported but does not guide us on how this can be done and does not allocate resources," she said.
"Hospitals do not have the resources to support doctors. It was clear that a dedicated program was needed and after the second wave, we were approached by doctors from the coronavirus wards who usually do not talk about emotional needs and asked for help. The main thing that came up in the questionnaire is that they do not know who to turn to in for emotional support," she said.
As part of the program, doctors and nurses had one on one meetings that dealt with burnout among other things.
"The burnout did not start with COVID," Barak said. "It has been there before and will be there long after the pandemic and this is an issue that must be addressed.
The problem is that we do not know what to do and there is also no magic solution. Treating burnout has to be done on many levels, from beefing up manpower to cutting down all the red tape to provide some solutions," Barak said.
First published: 14:20, 04.25.21