The tragedy of Reut Cohen, who died in her eighth month of pregnancy along with the twins she was carrying, has left behind difficult questions — including medical ones. Her family has raised the possibility of preeclampsia, but at this stage the official cause of death has not been determined, and it is unclear whether that was indeed the condition or whether another factor was involved. It is precisely this uncertainty, and the gap between severe symptoms and partial medical answers, that has brought renewed attention to one of the most significant and complex complications of pregnancy.
Preeclampsia is a condition that sometimes develops silently — and at other times erupts quickly. It can appear even in women with no clear risk factors, and its first signs are not always definitive. In some cases, the symptoms may resemble “normal” sensations of advanced pregnancy — pain, fatigue or discomfort — making early detection more difficult.
5 View gallery


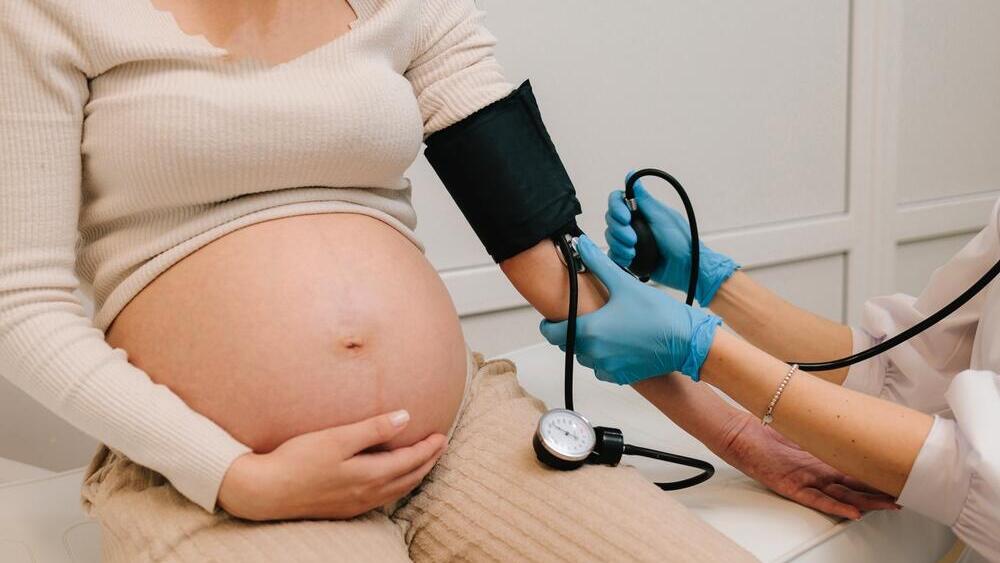
The silent killer: Sometimes fatigue or discomfort masks a major medical problem
(Photo: Yurii_Yarema / Shutterstock)
The current case, even without drawing conclusions, underscores how important it is to know the possible signs, understand when they deviate from the norm and, above all, know when to insist on further evaluation.
What is preeclampsia, and why is it complex?
“That is the million-dollar question,” says Dr. Orit Bernholtz, a specialist in high-risk pregnancy and endocrinology at Meuhedet Health Services in the Jerusalem district. “We know the disease mainly from its later stage — a woman with high blood pressure, protein in the urine and sometimes liver function abnormalities or a drop in platelets. Swelling, abdominal pain, blurred vision and even pulmonary edema can also appear — but that is actually the end stage of the disease.”
 Dr. Orit BernholtzPhoto: Private
Dr. Orit BernholtzPhoto: PrivateAccording to Bernholtz, it is important to understand that preeclampsia does not begin at the moment it is diagnosed, but much earlier. It is a process that begins in the early stages of pregnancy, following abnormal implantation of the placenta. “Today, we already know how to identify blood markers that can predict which women are at risk of developing preeclampsia later in pregnancy,” she explains.
Still, despite advances in detection, there is still no treatment that prevents the disease itself in its early stages. “What can be done is to identify women at risk and monitor them more closely, and sometimes provide treatment that reduces the risk — but not treatment that treats the preeclampsia itself,” Bernholtz stresses.
Who is at risk?
Preeclampsia is not rare and occurs in up to about 8% of pregnancies, though severe forms are less common. The risk increases with the number of risk factors, including pregnancy at an older age, pregnancy following fertility treatments and underlying conditions such as diabetes, high blood pressure or obesity. A first pregnancy at a very young age, as well as multiple pregnancies such as twins or triplets, also increase the risk of developing preeclampsia.
However, it is important to emphasize that preeclampsia can also develop in women with no known risk factors. “A woman can absolutely develop preeclampsia without us identifying a clear factor in advance,” Bernholtz explains, adding that there is also a hereditary component — not absolute, but one that can affect risk.
5 View gallery

Preeclampsia is a complication that can develop silently or rapidly, and can be difficult to detect in time
(Photo: Shutterstock)
In most cases, the disease appears in the third trimester, but it can also develop earlier. When preeclampsia appears at an early stage, it tends to be more severe and often requires premature delivery. This means not only increased risk for the mother, but also exposure of the newborn to complications of prematurity, making it a particularly complex condition that requires a delicate balance between protecting the mother’s health and trying to prolong the pregnancy as much as possible.
Signs, diagnosis and the challenge of detection
One of the major challenges with preeclampsia is that the symptoms are not always clear or definitive. Sometimes they can look like “normal” effects of advanced pregnancy, making them easy to miss. “Women do not always come in with all the features,” Bernholtz stresses. “And when there is only part of the picture, it can be very misleading.”
Still, there are signs defined as “red flags” that require immediate examination. The main symptoms include severe headaches, blurred vision, pain in the upper abdomen, shortness of breath and reduced urine output. “These are already hints of severe features of preeclampsia,” she says, “and in such situations it is very important to be examined as soon as possible.”
5 View gallery


When preeclampsia appears early, it sometimes requires premature delivery, exposing the newborn to complications of prematurity
(Photo: Shutterstock)
Diagnosis is based on a combination of blood pressure measurements, a physical examination and laboratory tests. A series of blood pressure measurements allows doctors not only to determine whether preeclampsia is present, but also to assess its severity. “A blood pressure of 160/110 or higher is already considered preeclampsia with severe features,” Bernholtz explains. Doctors also check for protein in the urine, and sometimes conduct a urine collection, alongside blood tests that include kidney function, liver function and platelet counts. Elevated kidney or liver function results, or a drop in platelets, may indicate a more serious condition.
The examination does not end there. In some cases, doctors also look for additional signs during the physical examination — such as significant tenderness or pain in the upper abdomen, which may lead to imaging tests such as an ultrasound to rule out rarer complications. At the same time, listening to the lungs can help detect pulmonary congestion, and if there are complaints of blurred vision or headaches, eye exams may also be performed to identify signs of cerebral edema.
One of the better-known and more complex complications is HELLP syndrome — a condition involving the breakdown of red blood cells, elevated liver enzymes and a drop in platelets. “HELLP can occur even without high blood pressure or protein in the urine,” Bernholtz stresses. “And because many other diseases can cause changes in liver function during pregnancy, it can be very misleading.”
5 View gallery


Pain in the upper abdomen is one symptom that may indicate preeclampsia and requires medical evaluation
(Photo: Shutterstock)
When it comes to imaging tests, it is also important to keep things in proportion. An MRI, for example, is not part of a routine preeclampsia workup. “Usually, it is not part of the routine evaluation,” she explains. “But a head MRI may be relevant if there is a change in consciousness or severe headaches, in order to rule out other dangerous conditions.” In recent years, an advanced blood test has also come into use that examines the ratio between certain proteins, sFlt-1 and PlGF, and can help doctors assess who is at higher risk of complications and determine how close monitoring needs to be.
Ultimately, the difficulty in diagnosis stems from the fact that the clinical picture is not always “orderly.” Certain symptoms can also fit other conditions — such as a viral infection or other liver problems during pregnancy — and therefore extra caution is sometimes required. “In medicine, there is never one symptom that fits only one disease,” Bernholtz notes. In cases where there is no clear answer, doctors sometimes decide to hospitalize the woman and continue monitoring to understand how things develop. Even then, she stresses, “unfortunately, there is never 100% certainty.”
The race to end the pregnancy
Preeclampsia is a disease that can change quickly — and sometimes deteriorate within a short time. “This is a disease that can deteriorate very quickly,” Bernholtz emphasizes. In such a situation, the most effective medical solution is delivery — ending the pregnancy. But in reality, that decision is far from simple, especially when the pregnancy is still at an early stage.
“When a woman arrives at an early week, we sometimes try to gain time to improve the fetus’ chances,” she explains. In such cases, doctors administer steroids to mature the fetus’ lungs, reducing the risk of severe illness and brain bleeding in the newborn, as well as magnesium intended to protect the fetus’ brain. Sometimes doctors try to “buy time” for about 48 hours to allow these treatments to take effect — but it is not always possible to wait, and the decision is made according to the condition of the mother and fetus at any given moment.
5 View gallery


In preeclampsia, the main and most effective treatment is delivery
(Photo: Shutterstock)
The decision of whether to keep the woman hospitalized or discharge her also depends on her condition. In cases of preeclampsia with severe features, women are not discharged. In milder cases, and under certain conditions, close outpatient monitoring may sometimes be enough. “Once there are severe features, a woman is not discharged home,” Bernholtz stresses.
The risks of preeclampsia are not minor — not for the mother and not for the fetus. For the mother, one of the known complications is seizures, but the risk does not end there. “There can also be brain hemorrhages, and preeclampsia is unfortunately also a cause of death,” Bernholtz says. In fact, in the Western world, diseases related to high blood pressure — including preeclampsia — are among the leading causes of maternal mortality.
The fetus is also at risk. Possible complications include placental abruption, intrauterine growth restriction and even intrauterine death. In other words, this is a medical condition that requires both rapid and careful attention. That is also the source of doctors’ central message: Do not ignore symptoms. “A woman who feels any of the symptoms must be examined,” Bernholtz stresses. Severe headaches, blurred vision, pain in the upper abdomen, shortness of breath or high blood pressure readings all require immediate medical evaluation.
Awareness is important not only during pregnancy, but also before it. Women who have had preeclampsia in the past should undergo evaluation before another pregnancy, identify risk factors that can be treated and begin early preventive treatment, such as aspirin. It is also important to stabilize conditions such as diabetes, high blood pressure and obesity in advance, and to be monitored as a high-risk pregnancy from the earliest stages.
And the woman herself is not the only one who needs to stay alert. Family members also play an important role in early identification of unusual situations. “If a pregnant woman looks like she is suffering in a way that does not fit the situation, or complains of severe headaches or something unusual, she should be taken to be examined,” Bernholtz says. Preeclampsia, she says, is a “misleading disease,” and sometimes insisting on another examination — even when everything seems normal — can make all the difference.


