Researchers at the Technion say they have developed an artificial intelligence model that can help determine whether early-stage breast cancer patients are likely to benefit from chemotherapy, a decision that has long posed a challenge for doctors and patients.
Chemotherapy after surgery can eliminate remaining cancer cells and reduce the risk of recurrence. However, for many patients it does not improve outcomes and can cause significant side effects, including long-term damage to the immune system. As a result, oncologists must weigh uncertain benefits against potential harm.
3 View gallery
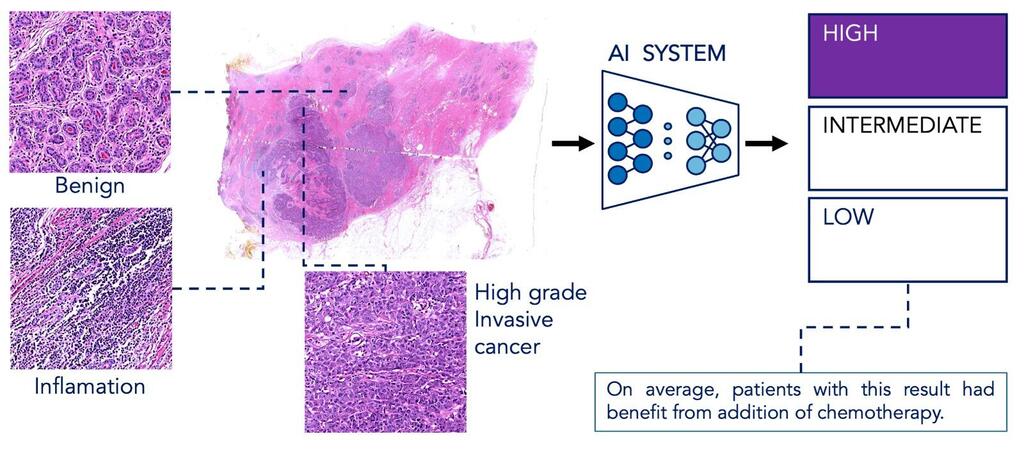

The artificial intelligence system analyzes the digital tissue sample of breast cancer taken at diagnosis
Each year, about 5,000 people in Israel — mostly women — are diagnosed with breast cancer. The figure is about 300,000 in the United States and roughly 2.3 million worldwide. Current tools, such as genomic tests like Oncotype DX, are used to estimate recurrence risk and chemotherapy benefit, but they are costly, take weeks to process and are not widely accessible. Their predictive accuracy is also limited.
The new AI-based approach, detailed this month in The Lancet Oncology and presented at the European Society for Medical Oncology conference, analyzes standard pathology samples taken at diagnosis. Using high-resolution images of tumor tissue, the system evaluates patterns linked to cancer behavior, including cell structure, division rates and signs of immune response.
“The system analyzes different regions of the tumor and its surroundings and identifies visual patterns associated with the biological behavior of the cancer,” said Dr. Gil Shamai, who led the study at the Technion’s Geometric Image Processing Laboratory.
Rather than relying on genetic profiling, the model extracts what researchers describe as a “visual signature” from stained tissue images. Prof. Ron Kimmel, who heads the laboratory, compared the method to identifying eye color by observation instead of analyzing genes.
The result is a numerical score generated within minutes that estimates both recurrence risk and the potential benefit of chemotherapy. The tool is intended to support, not replace, clinical decision-making.
Despite its performance, the system operates as what researchers describe as a “black box,” meaning its internal decision-making process cannot be easily explained. Still, the team reported that its predictions were consistent across different hospitals and patient populations.
The model was trained on large datasets of digital pathology images and further validated using samples from the TAILORx trial, a major randomized clinical study involving more than 10,000 breast cancer patients. Randomized trials are considered the gold standard in clinical research because they reduce bias in treatment comparisons.
Prof. Dvir Aran, a co-leader of the study, said the validation marks a significant milestone. “This is the first artificial intelligence model of its kind shown to predict the benefit of a treatment in breast cancer based on pathology samples,” he said.
Additional validation was conducted using patient data from hospitals in Israel — including Carmel, Emek and Sheba medical centers (Sheba is Israel’s largest hospital, located near Tel Aviv) — as well as institutions in the United States and Australia.
Researchers say the system could expand access to personalized medicine, particularly in developing countries where genomic testing is often unavailable. Because it relies on existing biopsy samples and standard digital scanning, it does not require additional procedures or specialized laboratory infrastructure.
The team is working toward clinical implementation in Israel and planning further trials in Brazil and India. They are also exploring applications for other cancers and treatment decisions.
The project involved collaboration with researchers and clinicians from multiple international institutions, including Dana-Farber Cancer Institute in Boston and the University of Chicago Medical Center. It was supported by several Israeli research initiatives, including the Israel Innovation Authority and the Israel Cancer Research Fund.
Researchers say AI-based tools like this could become a routine part of oncology care, helping tailor treatments more precisely while reducing unnecessary interventions.



