“You look down and see a parking lot, with arrows pointing to parking spaces, and you ask yourself, ‘Is this where people are treated?’ It’s truly horrific. I felt sorry for anyone who had to be hospitalized there. The air was suffocating, with almost no circulation. All the wards were crammed into one another. We were worried our son would catch some kind of infection. I told the nurse who admitted us that my son’s medical condition is complex, so he shouldn’t stay there long — but he said we should wear a mask and that there was no alternative. There was also a pregnant woman with us, who shouldn’t be sitting among sick people.”
This is how the mother of a patient who required treatment in an emergency room at a hospital in central Israel described the harsh conditions in an underground facility.
3 View gallery
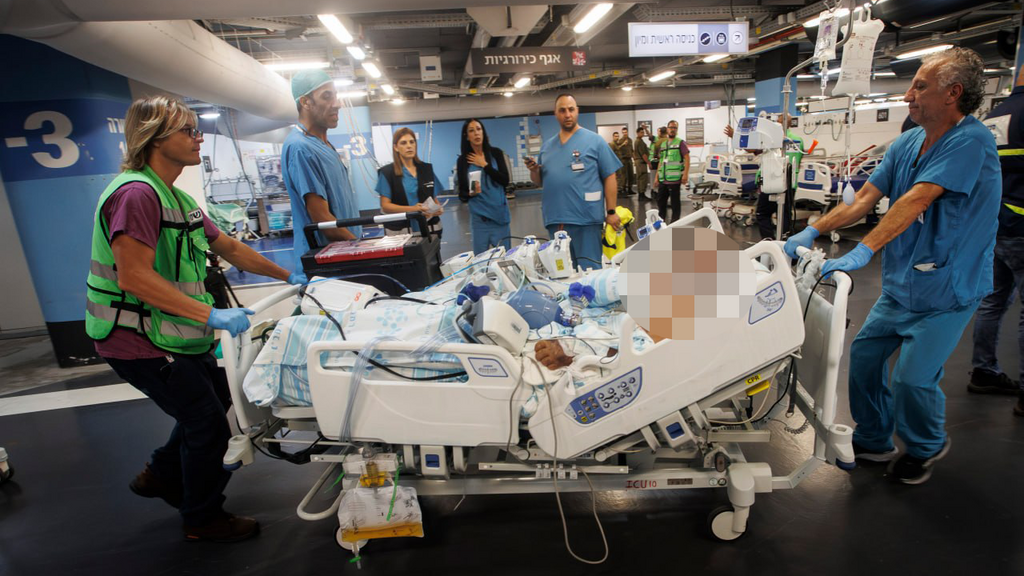

Patient moved to an underground complex at Rambam Hospital during war
(Photo: Gil Nehushtan)
Hospitals and Magen David Adom, Israel’s national emergency medical service, shifted to emergency mode at the start of Operation Roaring Lion.
According to the patient's mother, the difficult conditions were evident from the moment they arrived.
“The staff tried very hard, but it looked like they were thrown in there and told, ‘You have to work now.’ When we went inside, it was overwhelming — shouting, noise, shower curtains and tables. You looked up and saw cables running from one end to the other. We saw nurses sitting off to the side eating, without a moment of privacy. I was afraid to think how many mistakes could happen there. The only thing that calmed us was the sound of the early warning alert — we simply stayed seated. That’s really the only advantage of the place,” she said.
Hospitals and Magen David Adom move underground at the start of Operation Rising Lion
(Video: Spokespersons for the Ministry of Health, MDA, Sheba, Spokespersons for Rambam, Shabtai Yitzhak Idan, Spokespersons for Assuta Ashdodאשדוד)
For more than a month, hospitals across the country have been operating under emergency protocols: hundreds of patients have been moved to fortified underground complexes, and inpatient departments have been significantly reduced. The move was intended to address severe gaps in protection, but as time passes, the complex consequences of prolonged stays in such conditions are becoming clearer: no daylight, crowding, lack of privacy and an increased risk of infection.
About a week ago, a tuberculosis patient hospitalized in one such facility at Sheba Medical Center reportedly exposed nearly 2,000 hospital staff members and about 750 patients — including around 300 newborns and infants under the age of one, as well as immunocompromised patients. Those exposed were called in for evaluation, and some will require preventive antibiotic treatment for several months.
“The problem is that the underground complexes are not divided into separate rooms and wards, unlike standard hospitalization conditions,” explained Professor Yasmin Maor, head of the infectious diseases unit at Wolfson Medical Center and chair of the Israeli Association for Infectious Diseases.
According to Maor, those in the enclosed space breathe the same air, increasing the risk of airborne pathogens spreading — including measles, tuberculosis and chickenpox. “When exposure is continuous over time, the likelihood of infection rises significantly. It’s similar to what we saw with COVID: one contagious person in a large but enclosed, poorly ventilated space filled with people — the exposure is substantial.”
'I was speechless'
Maor noted that reducing hospital occupancy has left only the most severely ill patients — the elderly and immunocompromised — precisely those most vulnerable to infectious disease. “We are making efforts to prevent this, and the staff’s dedication is very high. But when one bed is touching another, it’s clear that the chance of bacteria passing from one patient to another increases,” she explained.
Maor added that, even in routine times, some hospitals suffer from poor infrastructure and overcrowding. “Every winter there are patients in the hallways. Some of these problems exist even in normal times — but now everything is accelerated.”
 Professor Yasmin Maor, head of the infectious diseases unit at Wolfson Medical CenterPhoto: Shlomi Mizrahi
Professor Yasmin Maor, head of the infectious diseases unit at Wolfson Medical CenterPhoto: Shlomi MizrahiLiat Sinai-Sades described the conditions in the facility where her mother, Esther Sinai, who has since died, was hospitalized in the early days of the war. “I heard the nurses talking among themselves about who would put up the curtains. During the two days we were there, there simply were no curtains," she said. "A staff member who came to change my 85-year-old mother’s diaper told her, ‘Close your eyes, that way you won’t see that people can see you.’ She was so embarrassed. Where is the most basic human dignity? Yes, it’s an emergency, but am I supposed to stand there with a towel and cover her? No one responded. I was speechless.”
“For months we’ve been hearing that hospitals are preparing — but in the complexes there is chaos,” she added. “Staff were going up and down dozens of times to bring equipment. I don’t understand how a country that has experienced so many wars is not properly prepared. It’s not a big story — to put 500 plastic chairs on the side. Even the cleaning carts kept going up and down. Why aren’t they there permanently?” After two days in the facility, her mother asked to return home. “She said: ‘I can’t take it anymore,'” Sinai-Sade said.
3 View gallery
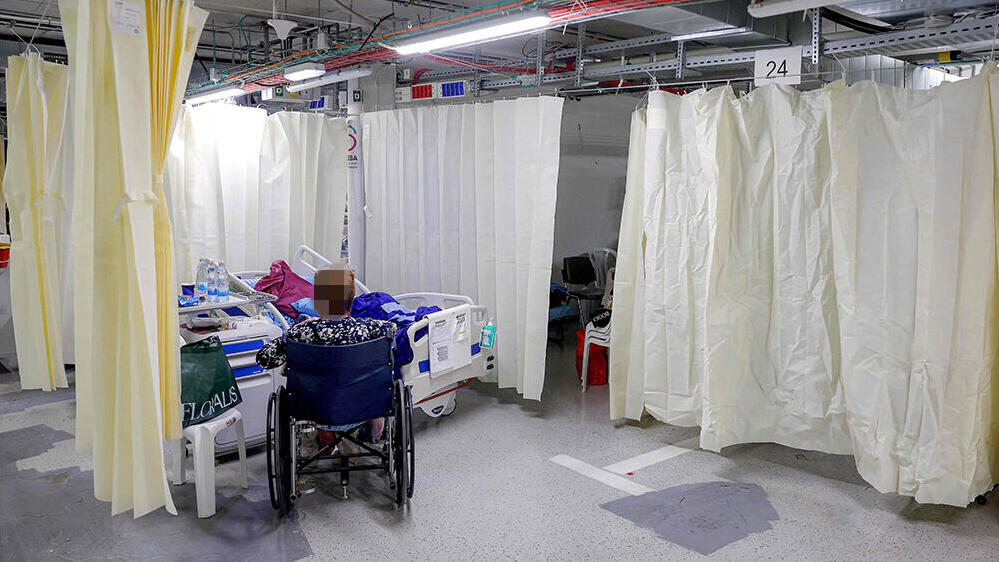

Hospitalized in the underground complex at Sheba Medical Center Tel Hashomer
(Photo: Jack Guez / AFP)
The mother of the emergency room patient also noted accessibility problems. Her 25-year-old son uses a walker, but the site had only stairs leading down to the facility. “We just stood there wondering what to do.” After a long walk, they reached an accessible entrance — but encountered a steep descent. “We found a wheelchair thrown to the side, but they told us to wait for someone to come get us. We explained to the guard that our son was injured and had a head wound, and only then were we taken to the elevator.”
She stressed that the issue affects not only people with disabilities, but also elderly patients and those who struggle to descend stairs.
'Conditions from old films'
“The whole concept originates in a fundamental failure,” Maor said. “The missile threat was known in advance, and nothing was done to adequately fortify hospitals. It comes back to the question of what the state chooses to invest in.” According to her, the physical conditions are difficult for both patients and staff. “It’s very unpleasant to stay in such a space for a long time — these are conditions from old films, not a modern hospital.”
3 View gallery


Ichilov Medical Center emergency hospital
(Photo: Jenny Yerushalmi and Miri Getaniu, Ichilov spokespeople)
A senior physician at one hospital reported that many staff members working in the facility complained of recurring headaches. “Gas concentration tests found that carbon dioxide levels were high. This wasn’t checked until staff complained. After the test, steps were taken to improve circulation," he said.
He added another concern: “Once you take staff out of their familiar environment, their clinical instincts are disrupted — and that can also affect the quality of care. In a few months, we will need to examine whether there was excess mortality. I wouldn’t be surprised if we see the impact of this period.”
The concern is heightened by a measles outbreak in Israel that has so far claimed the lives of 17 children. In recent weeks, several children were diagnosed with measles only after being hospitalized in fortified complexes alongside other patients. One of them, a 17-year-old boy, died after being diagnosed while staying in an underground facility at Schneider Children’s Medical Center.
“Measles is highly contagious, and patients need airborne isolation in negative-pressure rooms — which are already in short supply even in normal times,” explained Professor Galia Rahav, an infectious disease specialist. “Even if patients are isolated, when there is a siren they must be moved to a protected area — and during that transfer many others may be exposed.”
“Not long ago I saw a baby arrive at the emergency room with diarrhea, and no one thought it was measles — and rightly so,” Rahav said. “Only after several hours did a rash appear, and he was diagnosed. By then, there had already been in contact with other patients. It’s a shame we didn’t reach higher vaccination rates.”
 Professor Galia Rahav, an infectious disease specialistPhoto: Private album
Professor Galia Rahav, an infectious disease specialistPhoto: Private albumRegarding the tuberculosis case at Sheba, she said: “There aren’t many TB cases in Israel, but an event like this can lead to a larger outbreak. Fortunately, the disease develops slowly, and illness can be prevented if action is taken in time.”
Rahav emphasized that conditions are also difficult in geriatric hospitals, where there has been a rise in cases of RSV and COVID-19, as well as gastrointestinal infections including norovirus. “Hospitals have purchased portable sinks, but it’s very difficult to maintain all hygiene rules. Everyone is under pressure, the focus is on protection, and infection prevention is pushed aside — that’s something I hear often. When we leave the parking structures, I am sure we will see more infections with resistant bacteria. That’s what happened after October 7,” she said.
The Health Ministry is aware of the difficulties, but its position remains clear: due to the security threat, hospitals will continue to operate under this format as long as necessary.
“We are balancing between meeting Home Front Command requirements and protecting hospitals — especially when Iran is targeting the health system as a strategic objective — and maintaining quality of care, patient safety and infection prevention,” an official said. “The conditions are far from ideal, for both staff and patients, but we are monitoring the situation closely and do not currently see extreme crises.”



