According to estimation, hundreds of Israelis are hospitalized for food poisoning every year. It can manifest as stomachaches, vomiting, and diarrhea, but sometimes food poisoning can deteriorate to life-threatening situations, especially among vulnerable populations such as infants, the elderly, the immunocompromised, and pregnant women.
More Stories:
Foodborne infections are very common worldwide, particularly in places where the necessary conditions for storage, preparation, and serving of food aren’t well maintained.
Since the incident of a Salmonella outbreak in a breakfast cereal plant in Israel in 2016, the Health Ministry has intensified inspections, and one business was closed almost every week after bacteria or parasites were found in food products.
Food contamination can occur at home or restaurants, at the workplace, or even on production lines. Not much is required in order to contaminate an entire line with harmful organisms.
In severe cases, especially in infants, the elderly, or people with compromised immune systems, bacteria can enter the bloodstream and cause a systemic infection (sepsis) that can be life-threatening.
Bacteria require moisture and warmth to grow, and with favorable conditions, a single bacterium can multiply exponentially, multiplying to millions within 8 hours and to billions within 12 hours.
10 View gallery


Topolopompo restaurant in Tel Aviv where a diner was evacuated to a hospital due to food poisoning
(Photo: Yuval Chen)
Here are some of the most common bacteria found in food, their effects on the human body, possible treatments, and ways to prevent contamination.
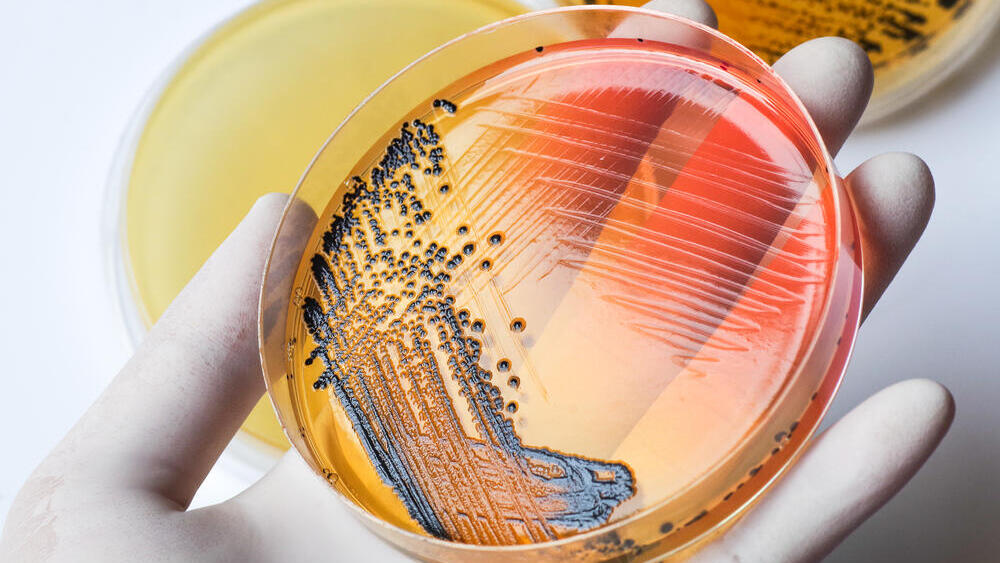
Salmonella
Salmonella is a bacterium from the Enterobacteriaceae family. There are approximately 2,000 strains of Salmonella, but only about a tenth of them are harmful to humans and cause illness.
Under a microscope, the bacterium appears with a flagellum that allows it to move, and it has a capsule that aids in its resistance and contamination capabilities. Salmonella can be contracted through almost any contaminated food, especially dairy products, eggs, and meat.
Symptoms usually appear within 6 to 72 hours after exposure and typically include abdominal pain, nausea, vomiting, fever, diarrhea, and fatigue. In rare cases, the bacterium can enter the bloodstream and cause a systemic infection that can be life-threatening.
The Health Ministry oversees salmonella detection, and food companies in Israel are also required to test for it. To prevent its growth, it’s important to store food at a temperature below 5° C (41°), avoid washing eggs because that could lead to the penetration of the bacterium through the shell, and ensure thorough cooking of meat.
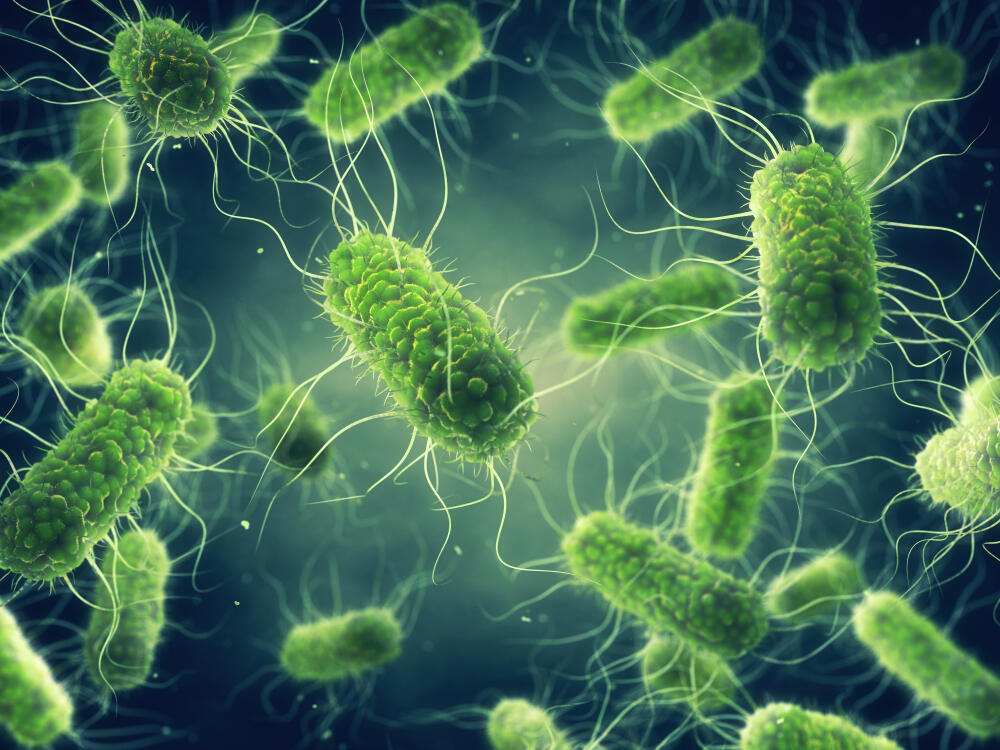
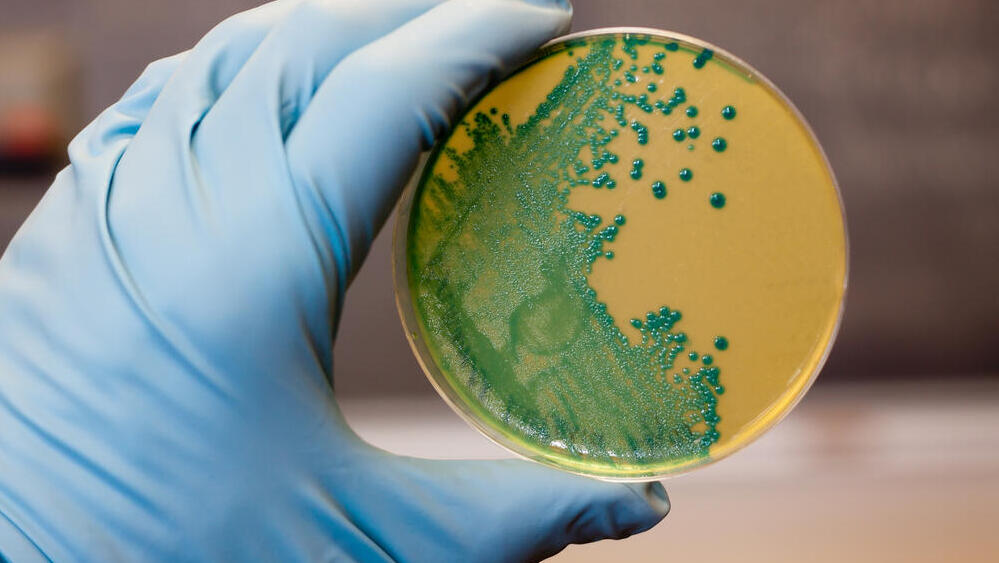
Shigella
Shigella is a fecal bacterium that has been known since the late 19th century. At the time, it caused severe intestinal diseases in Japan and was discovered by Japanese researcher Kyoshi Shiga, who gave it his name.
It can be transmitted through various means: contact with the infected fecal matter or with surfaces or animals that were contaminated by fecal matter, or via consumption of food that has been in contact with an infected person.
Symptoms appear within one to two days after infection and include diarrhea, high fever, and abdominal pain. The illness can last up to a week. Some patients may develop complications such as meningitis, sepsis, muscle contractions, or damage to red blood cells known as hemolytic-uremic syndrome.
The diagnosis of this bacterium, similar to other fecal bacteria, is performed by culturing a stool sample sent to the laboratory. The main treatment includes increased fluid intake with sugars and salts.
If an infant was infected, a doctor may recommend an electrolyte solution in addition to regular nutrition. This solution replenishes the body with salts like sodium and potassium, as well as glucose.
Antibiotic treatment is recommended even if contamination is only suspected, out of concern for possible neurological damage. The accepted treatment in Israel is Rifaximin administered by injection.
To prevent infection, it’s important to maintain personal hygiene, especially in cases where a family member was already infected. It’s also important to wash your hands before eating, after changing a baby's diaper, after using the restroom, and before handling food.
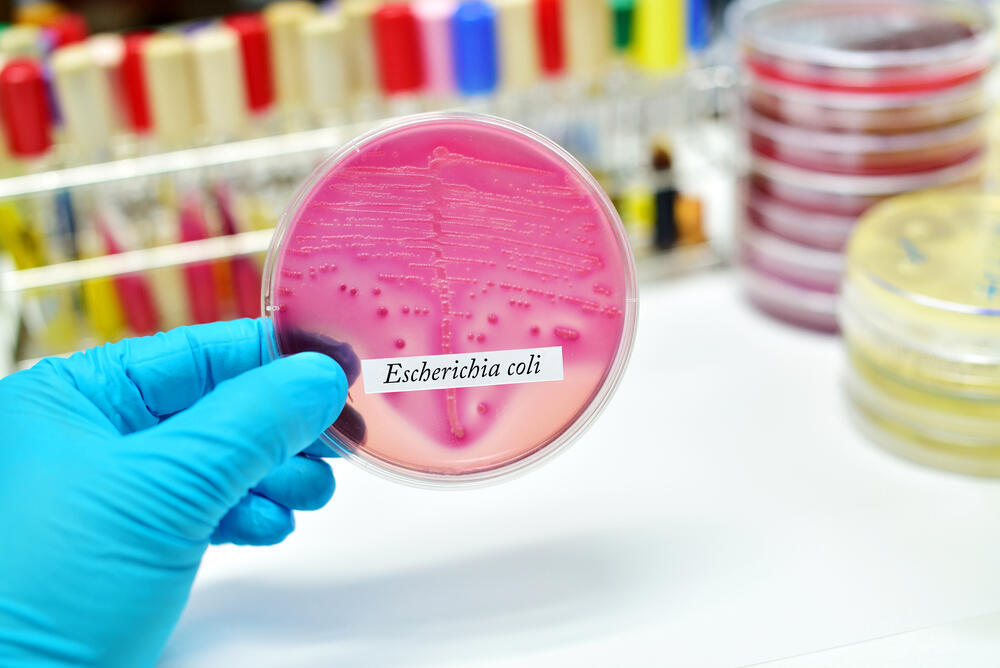
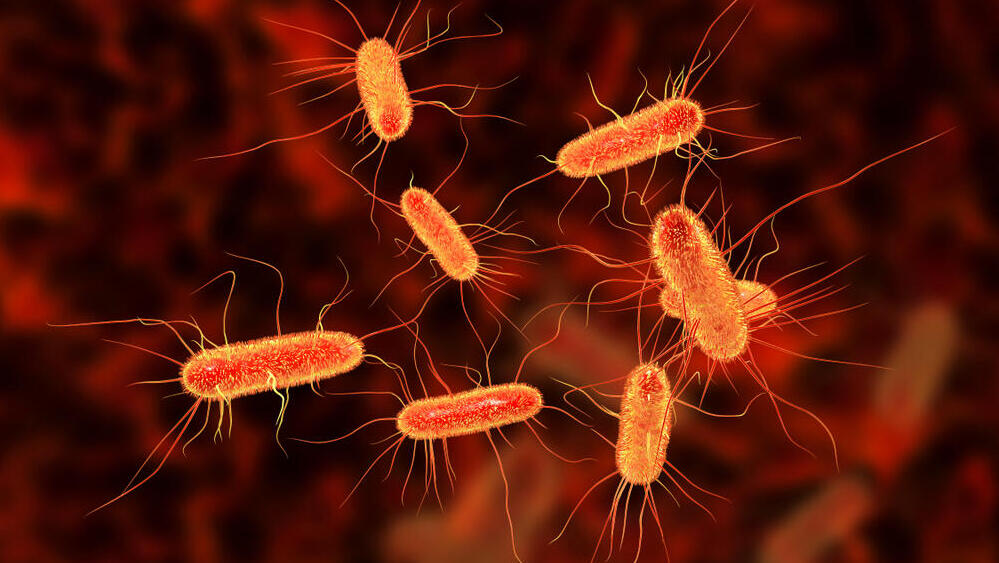
Escherichia coli (E. coli)
The bacterium was discovered in 1885 by researcher Theodor Escherich, who named it after himself. Escherichia coli, also known as E. coli, is a fecal bacterium that lives in the intestines.
It receives nutrients and protection in the gut and assists digestion by secreting enzymes that break down some of the nutritional components that the body cannot digest. but it can cause severe diseases.
The bacterium has several dangerous strains. One of them produces a toxin similar to those produced by Shigella and Salmonella bacteria and can cause severe intestinal disease. If it passes from the intestines to the urinary tract, it can cause inflammation there.
It can also pass into the abdominal cavity through a tear in the colon, as seen in severe appendicitis, where it can cause severe inflammation called "peritonitis."
Symptoms appear within one to two days after eating contaminated food and include abdominal pain, vomiting, diarrhea, and urinary tract infection. Certain strains can cause kidney damage and even death. In rarer cases, a newborn baby can become infected with the bacterium after birth.
If concerns of infection arise in a high-risk patient or someone already suffering from a severe illness, antibiotics that kill the bacterium within days can be administered. Deaths as a result of infection are very rare in Israel, but infection isn’t uncommon, and dozens of infants are infected with it every year.
To prevent infection, meat should be cooked at a temperature of at least 63°C ( 145°F) use only pasteurized milk, and store food products according to instructions on the lable.
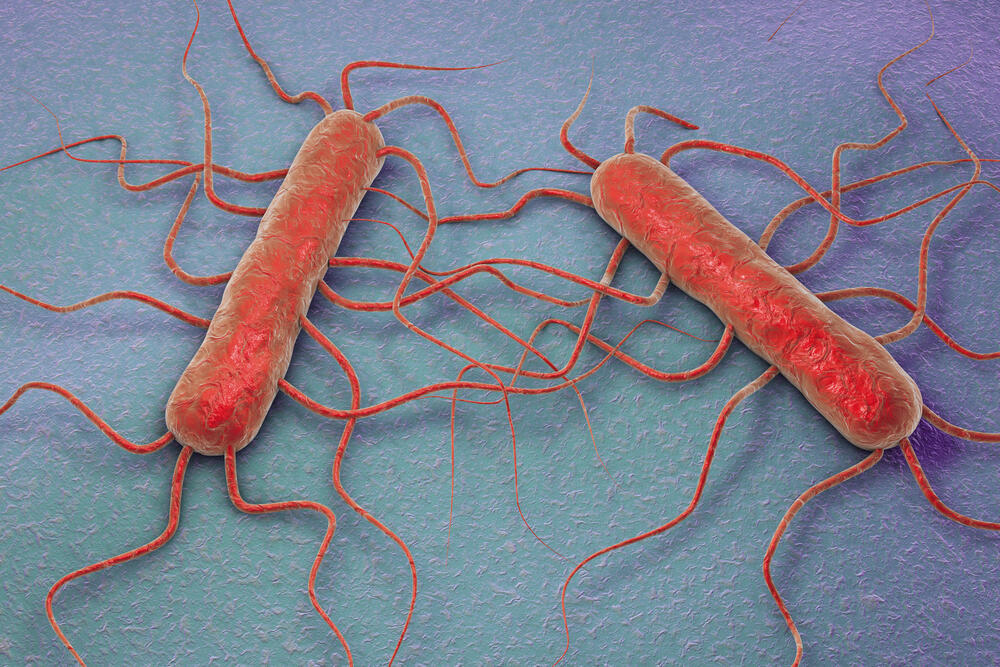
Listeria monocytogenes
This is an environmental bacterium found in soil and various foods. It has unique characteristics that allow it to grow and multiply in cold conditions –such as a refrigerator at 4° C (39°F) - and in foods with high amounts of salt, such as smoked products.
Foods that have been found at risk of being contaminated include smoked fish and meat, unpasteurized dairy products, improperly washed vegetables, and other food products that have undergone insufficient heat treatment.
Food that has been properly cooked but cut on a board that has not been thoroughly cleaned, can also become contaminated.
Symptoms appear within three days to two months of consuming contaminated food and resemble flu-like symptoms such as fever, fatigue, nausea, vomiting, and diarrhea.
In severe cases, the bacteria can enter the bloodstream and cause serious complications, such as blood infection (sepsis), meningitis (especially in children and infants), miscarriage, premature birth, severe damage to the fetus, pneumonia, and pericarditis.
Listeria is considered a highly antibiotic-resistant bacterium. Treatment involves ampicillin or co-trimoxazole.
To prevent infection, it’s recommended to cook animal products such as poultry and fish at a temperature of at least 72° C (161° F.) Avoid purchasing meat, fish, and unpasteurized dairy products from questionable sources.
It’s important to wash your hands with soap and water before and after food preparation, to wash vegetables and fruits with soap and water, and to avoid consuming products that have been in the refrigerator for a long time or have expired.
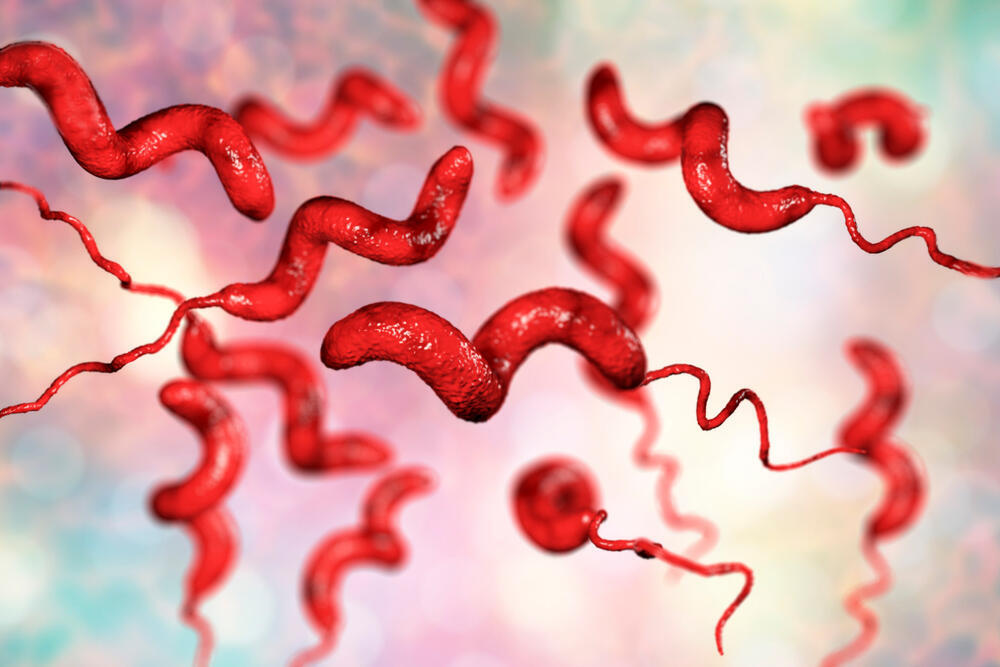
Campylobacter jejuni
Campylobacter is a fecal bacterium that resembles a spiral and was discovered in the late 19th century, but only in 1977 was it found to cause disease. It is naturally found in the digestive system of young animals and birds and is usually transmitted to humans through undercooked meat or poultry.
Symptoms appear within one to eleven days of consuming contaminated food and are similar to those caused by other intestinal bacteria, primarily abdominal pain and diarrhea with or without vomiting.
Pregnant women are at a higher risk of contracting Campylobacter from contaminated food. Infection in pregnant women can be dangerous and may lead to miscarriage, stillbirth, or infant death following birth.
Treatment is usually palliative, including increased fluid intake or intravenous fluid administration.
In severe cases, antibiotics from the cephalosporin or macrolide groups can be used. To prevent infection, it is recommended to cook food at a temperature of at least 48° C (118° F) maintain personal hygiene, and avoid purchasing food from questionable sources.