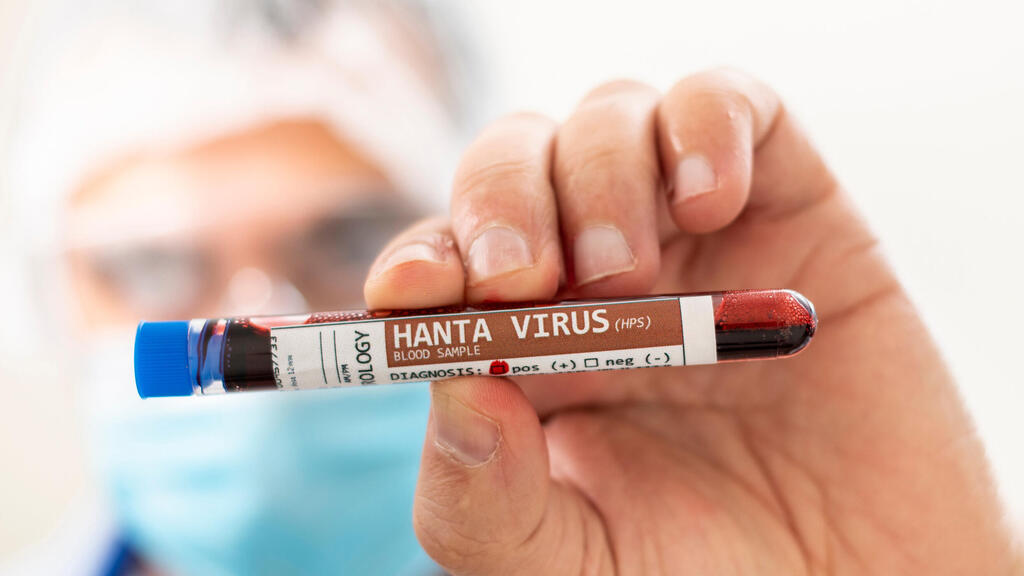
It started like a movie we have already seen: A deadly disease that passes from animals to humans breaks out aboard a cruise ship. The disease, for which there is no vaccine or cure, begins with flu-like symptoms. Three passengers die, others are infected, the entire ship is quarantined, words like “Diamond Princess” and RNA rise from the depths of memory, and an old-new fear returns: Are we facing the start of a new global pandemic?
The outbreak of hantavirus aboard the MV Hondius last month does indeed evoke bad memories. But we can relax: Despite the similarities and despite very high mortality rates — 30% to 50% of those infected — this is not a new pandemic. Hantavirus is relatively rare, harder to contract — one must be directly exposed to secretions from infected rodents or inhale airborne particles from them, charming — and harder to transmit to others. In addition, surprisingly, there were no Israelis aboard the Hondius, and the whole thing largely passed us by.
The virus was named after the Hantan River in Korea, where the first outbreak was documented among soldiers in the 1950s. It is a family of viruses carried mainly by rats and mice, though bats, moles, reptiles and fish have also been found to be carriers. The carriers do not become ill, but shed the virus through urine, droppings and saliva. Although the virus exists on every continent where rodents live, only about 10,000 cases are reported worldwide each year. For comparison, there are more than 11 million measles cases. In Israel, only one hantavirus case has been reported so far: In December 2025, a person returned from Eastern Europe with the virus, but it was a different strain from the one on the ship and is not transmitted from person to person.
“Hantavirus is at the bottom of the list of pandemic threats,” says Professor Tal Brosh, director of the Infectious Diseases Unit at Assuta Ashdod Public Hospital and head of the Health Ministry’s epidemic response team. “At the top of the list is a new coronavirus strain. After that, avian flu. It is a disease that can be deadly. As of today, it is not transmitted between humans, but the risk is a virus that acquires the ability to pass from person to person.”
Still, before we forget the whole thing and return to our usual lack of normalcy, hantavirus is a good opportunity to ask whether Israel is prepared to face the next pandemic, which everyone agrees is only a matter of time. The answer is not comforting: Dealing with a pandemic is a multifront campaign. It is not “just” a medical matter, but a social, economic, political and even geopolitical challenge, since a pandemic is by nature global. On all these fronts, unsurprisingly, we are in trouble.
A part-time minister
Israel’s health system is a kind of medical miracle in itself. National health spending in Israel is among the lowest in the OECD by a wide margin, with severe shortages of beds, infrastructure, personnel and professional reserves; gaps between the center and the periphery; medical teams worn down and stretched to the limit after two and a half years of emergency and wartime work; a quarter-time health minister; a Health Committee that barely convenes — and perhaps that is for the best, since under Knesset lawmaker Limor Son Har-Melech it has become a spectacle of shouting and bullying; a completely neglected public health field; long waits for tests; and more.
And yet, despite all this, Israelis are healthier and live longer: With an average life expectancy of 83.8 years, we rank fourth in the developed world. That is mainly thanks to the fact that we have excellent doctors and nurses who give everything. But the fact that it has worked until now does not mean it will keep working forever. Even a medical miracle comes to an end. A starved system will eventually collapse.
A starved and weakened system, explains Professor Itamar Grotto, a public health expert and former deputy director-general of the Health Ministry, has a short memory. “When there is no continuous, constant preparedness and the issue falls off the public radar, the system’s readiness declines and professional capabilities deteriorate. Some of the knowledge disappears, and you have to start from scratch.” Our luck, Grotto says, like most of the doctors I spoke with, is that “the system will know how to work in an emergency.” Again, we rely on the human factor and its motivation instead of giving the system adequate conditions. In the end, that is another way of saying, “It’ll be fine.”
At the start of the month, the State Control Committee held a discussion on “pandemic influenza and the procurement of a long-term stockpile of antiviral drugs.” At the discussion, representatives of the State Comptroller’s Office presented reports on handling emerging and reemerging diseases, including a broad pandemic outbreak, public vaccination and the effect of COVID on public attitudes toward routine vaccines.
5 View gallery


Medical team with protection leaves the hantavirus-infected MV Hondius
(Photo: Hannah McKay/Reuters)
The discussion and the reports present a fairly clear picture: The Health Ministry, health maintenance organizations and hospitalization system are not fully prepared for a pandemic outbreak. In general, when digging through the various state comptroller reports and other studies dealing with Israel’s preparedness for the next pandemic — and not only that — one finds a familiar pattern, far too familiar: The flaws are known, but not always addressed. Important lessons were learned from COVID and are being successfully implemented, but many others were not.
How incomplete is the preparedness? Dr. Or Krieger, deputy head of the Health Ministry’s Public Health Division, revealed at the discussion that, although the preparedness plan requires the state to stock antiviral drugs sufficient for a quarter of the population, the current stockpile is enough for only 1% of us.
This is, of course, a significant expense. “We are not a very rich country,” Brosh says. “The amount of medicine we have today in case of a pandemic outbreak is not enough. I am, of course, in favor of buying drugs, but the question of whether the state should invest in that specifically or elsewhere is a legitimate one.”
And as if that were not enough, the current situation, in which Health Minister Haim Katz simultaneously holds three other portfolios — tourism, construction and housing, welfare and social security — harms the system’s efficiency, creates a managerial failure, leads to unprofessional decision-making and neglect of long-term planning, according to the Association of Public Health Physicians. This is another aspect that shows how much a strong, professional and functioning health system does — or does not — matter to Israel’s political leadership, and how much it does — or does not — matter to them to place at the top of the system a serious person who deeply understands health needs. And then they tell us health is what matters most.
That says a lot. The status of professionals in Israel is being steadily eroded — after all, they are all part of the deep state — in favor of political appointments, sometimes more successful, sometimes less. “Health is not on the list of priorities. Not in routine times and not in emergencies — but then it becomes more obvious,” sums up Professor Hagai Levine, chairman of the Association of Public Health Physicians in Israel.
A catastrophic mistake
But the two truly major challenges facing the health system and the State of Israel as a whole in the event of a pandemic outbreak are actually nonmedical challenges, and they are the ones that could tip the scales against us.
The first, cited by Brosh, Levine and others, is the fact that a pandemic is, by nature, global — and the response to it must also be global. No man is an island. But it is no great secret that Israel’s standing in the world is eroding, not to say being ground down to dust.
“This is a serious problem,” Levine says. “Once we could talk to everyone. Today, if you want contact with health bodies around the world, Israel is no longer a priority. Our communication capability has been damaged. MK Limor Son Har-Melech wants to disconnect us from the World Health Organization. That means being cut off from all global databases. We are seeing cracks in our ability to cooperate with international bodies.”
“The desire of certain political elements to disconnect from the World Health Organization is a mistake that does not advance us in terms of pandemic preparedness,” Brosh agrees. “It may be that some of the things said by those who support disconnection are true, but international cooperation is very important. You have to be connected to the world. In my view, it would be a catastrophic mistake. I hope we do not get there. It means that the next time we need to buy vaccines, we may not be as attractive to companies that want to sell to us.”
And now we arrive at the main course. The most important challenge the next outbreak will place before us is public trust. It is simply impossible to fight a pandemic without public compliance. But public trust in almost all state institutions, including the health system — and not only in Israel — is in a deep crisis and at an unprecedented low. Imagine that tomorrow an announcement goes out calling on the Israeli public to get tested or avoid gatherings. Who would listen, and to whom? Who would believe it? Whom would we obey? No one believes anyone anymore. Everyone with a Facebook account has become an epidemiological expert.
“There is undoubtedly a significant break in public trust,” Brosh agrees. “And it is connected to COVID. People do not want to hear from scientists, they do not believe doctors or government bodies. There has been a change in people’s attitude toward facts. Scientific truth does not beat the personal opinion of someone with many followers.”
5 View gallery
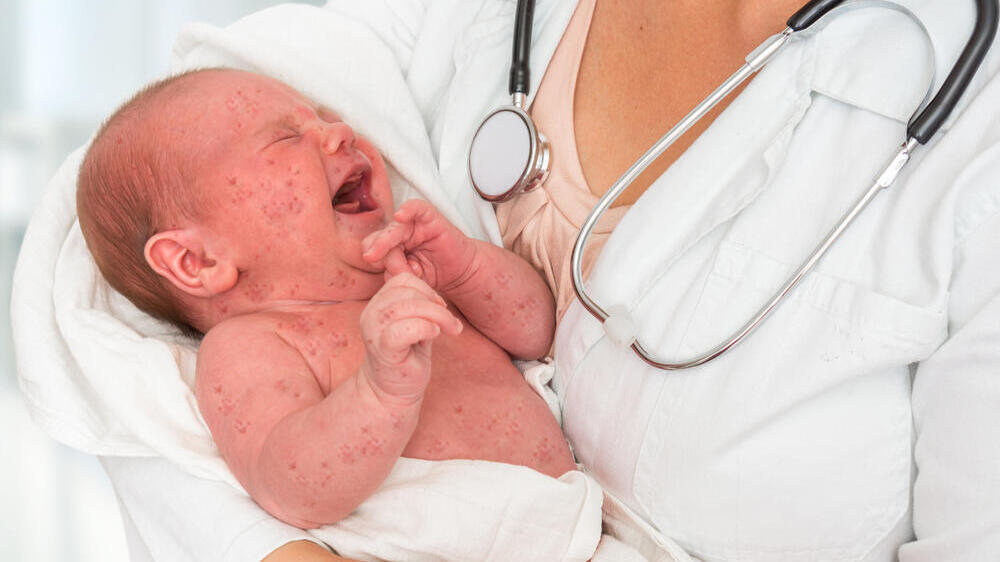

Seventeen people in Israel have died of measles in the last year
(Photo: Shutterstock)
There is no need to wait for hantavirus or imagine the system’s lack of preparedness and the public’s lack of trust in the next outbreak. Other outbreaks of zoonotic diseases — those transmitted from animals to humans — in Israel in recent years do not bode well either. In 2024, while we were busy with the war in Gaza, there was an outbreak of West Nile fever in central Israel after a malfunction at a wastewater treatment plant in Ramat Hasharon. More than 900 people were infected, 73 of them died, before the state woke up. I admit I had not heard of it at all.
And, of course, measles. For more than a year, Israel has had a measles outbreak among populations that do not vaccinate. Since April of last year, more than 3,600 patients have been diagnosed, 90% of them toddlers and children, and the vast majority unvaccinated — in addition to at least 10,000 other Israelis who were infected but not diagnosed. Seventeen people have died of the disease to date. “These are not numbers we should be seeing in a Western country,” Grotto says. “It is very worrying.”
“Measles,” Brosh says, “demonstrates how public trust is one of the most significant problems today and in the near future in dealing with such events. There is an erosion in vaccination, and measles is raging among the unvaccinated.”
In April, the medical journal JAMA Health Forum published an article by Professor Itai Shavit of Hadassah Hospital, Dr. Giora Weiser of Hadassah and Tel Aviv University and Dr. Oren Feldman of Sheba Medical Center, under the headline “The Severity of Israel’s Measles Outbreak — Cause for Concern.” In the article, the authors note that “the measles event is an expression of a deep injury to public trust,” no less than it is a medical issue. “The measles outbreak,” they wrote, “highlights how social, cultural and communication failures can erode achievements built over decades in Israel’s public health field.”
In a normal country — for anyone who remembers such a thing — the deaths of 17 children could not pass under the radar. But here, it passes quietly. At that same State Control Committee discussion mentioned earlier, it emerged that the Health Ministry has no operating procedure regulating the required activity during a measles outbreak. This is despite the fact that more than a year has passed since the outbreak began. What’s the rush? If Israel’s handling of the latest measles outbreak teaches anything about its ability to deal with the next pandemic, we are in trouble. But on the other hand, it will probably be fine.
'Working to ensure preparedness'
The Health Ministry said in response: “The ministry is conducting a professional situation assessment and continuously monitoring developments regarding hantavirus morbidity. The ministry is prepared in terms of diagnostic capabilities and testing stockpiles and works routinely to ensure preparedness for scenarios of emerging diseases and pandemics. Israel maintains ongoing working ties with the World Health Organization and other international health bodies.”